Brief Report - (2023) Volume 14, Issue 2
Abstract
Background: Tuberculosis remains a serious public health problem in the Gambia, 6th top cause of DALYs (Disability-Adjusted Life Year). Treatment outcome serves as a tool to control the quality of tuberculosis treatment provided by the health care system. The global epidemiology of tuberculosis has been shaped in recent decades by HIV/AIDS, urbanization and poverty. The majority of survey detected TB cases (95%) were new and not on treatment at diagnosis (Gambia Health Policy 2021-2030).
Methods: The study is a retrospective cross-sectional secondary data review aimed at analyzing existing programmatic tuberculosis data extracted from the DHIS2.
Results: A total of 4109 TB cases (Extrapulmonary and Pulmonary) were recorded in DHIS2 for the period 2017 to 2021, of which 3,349 (81.5%) were pulmonary TB cases, males accounted for 59.9% while Western Health Region one which has about 50% of the national population accounted for 51.1% of the total number of cases 2099 (51.1%). A total of 5491 cases were reported for treatment outcome, this is higher than the number of active cases for the period in review which could be because data from the previous year reported in the new year. Out of this 575 (10.5%) completed treatment whiles 4720 (86%) were cured. During the period, a total of 3472 HIV positive TB co-infections were reported of which 36.1% (1290) were on ART, 9.9% (353) were cured and 4.0% (died).
Conclusion: We realize that there is a high turnout rate for treatment outcome especially for those that complete their treatment and those that are cured.
Keywords
Tuberculosis, Treatment outcome, Co-infection, HIV, District Health Information System 2 (DHIS2)
Introduction
Tuberculosis remains a serious public health problem in the Gambia, as the 6th top cause of DALYs. In 2019, Tuberculosis (TB) was the leading cause of death from an infectious agent accounting for 1.2 million deaths among HIV-uninfected people and 208,000 deaths among HIV-infected individuals globally (Baluku JB, et al., 2022).
In the WHO African region, where the burden of HIV-associated TB is highest, 85% of TB patients had a documented HIV test result. Overall, in 2020, 88% of TB patients known to be living with HIV were on ART (WHO fact sheet, October 2021). Africa accounts for ¼ of the global burden out of which 32% are co-infections with HIV, and national burden of TB is 128/100,000 representing a sharp decline from 2013 which was 490/100,000.
The majority of unsuccessful outcomes were attributed to death and of defaulter rate. HIV co-infection and retreatment were significantly associated with an increased risk of unsuccessful treatment outcomes compared to HIV negative and newly diagnosed TB patients, respectively. TB treatment success rate was in Africa was 79% below the WHO defined threshold of 85% with significant variation across countries (Teferi MY, et al., 2021).
Treatment outcome serves as a tool to control the quality of tuber- culosis treatment provided by the health care system. The global epidemiology of tuberculosis has been shaped in recent decades by HIV/AIDS, urbanization and poverty. Despite the availability of effective treatment, tuberculosis (TB) remains a major cause of morbidity and mortality, particularly in the developing world (Harper M, et al., 2003). Non-adherence to anti-TB treatment may result in the emergence of Multidrug Resistant TB (MDR-TB), prolonged infectiousness and poor TB treatment outcomes (Tesfahuneygn G, et al., 2015; WHO, 2021). In previous studies, patient-related factors including feeling better, forgetfulness, lack of knowledge on the benefits of completing a treatment course, running out of drugs at home, distance to the health facility, HIV seropositivity, alcohol abuse, use of herbal medication, stigma and male gender were significantly associated with non-adherence to an anti-TB treatment (Tesfahuneygn G, et al., 2015).
We conducted this study to describe pulmonary and extra pulmonary treatment outcomes in Gambia between 2017-2021.
Methodology
Study setting/area
Gambia is located on the West African coast and extends about 400 km inland, with a population density of 176 persons per square kilometer (WHO, 2021). The width of the country varies from 24 to 28 kilometers and has a land area of 10,689 square kilometers. According to the Population and Housing Census (IHSN, 2013) projections, the population is estimated at 2.4 million in 2020, 50.7% are females with annual growth rate of 3.1%.
The population size is set to reach 2.8 million in 2025. The crude birth rate is 46 per 1000 population while the total fertility rate is 4.4 births per woman (WHO, 2021). The high fertility level has resulted in a very youthful population structure. Nearly 44% of the population is below 15 years and 19% between the ages 15 to 24. Average life expectancy at birth is 61.5 years overall with females constituting 62.3 and males 59.6 years (WHO, 2021).
TB is diagnosed and managed at 41 DOT sites across the country and these sites are in the hospitals, major and minor health facilities. There are regional leprosy TB officers at all the seven regional health directorates who support and coordinate TB control activities in their various regions.
Study design
We reviewed tuberculosis surveillance data obtained from the DHIS2. Data source and analysis we reviewed TB data obtained from the DHIS2 covering 2017-2021. We extracted data on TB types, and different types of categories of bacteriologically confirmed treatment outcomes. We validated, tabulated and analyzed data using Microsoft Excel (WHO, 2021).
Results
A total of 4109 TB cases (Extrapulmonary and Pulmonary) were recorded in DHIS2 for the period 1st January 2017 to 31st December 2021, of which 3,349 (81.5%) were pulmonary TB cases, males accounts for 59.9% while Western Health region one which has about 50% of the national population accounts for 51.1% of the total number of cases 2099 (51.1%). A total of 5491 cases which were reported for treatment outcome as illustrated in Figure 1 below, out of this 575 (10.5%) completed treatment, while 4720 (86%) were cured.

Figure 1: Proportion of TB cases with an outcome in the Gambia
from 2017-2021
Note:  : Pulmonary Tuberculosis (PTB);
: Pulmonary Tuberculosis (PTB);  : Extrapulmonary Tuberculosis (EPTB).
: Extrapulmonary Tuberculosis (EPTB).
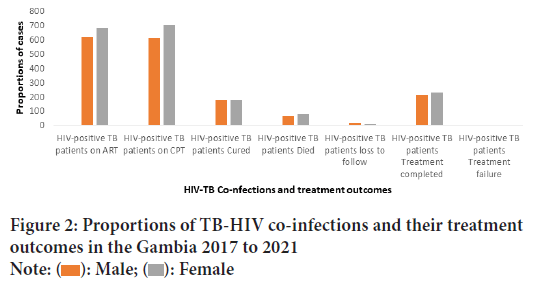
During the period, a total of 3,472 HIV positive TB co-infections accounting for 84.5% of the total reported cases during the period were reported of which 36.1% (1290) were on ART, 9.9% (353) were cured and 4% (died) as shown in Figure 2below.
Figure 2: Proportions of TB-HIV co-infections and their treatment
outcomes in the Gambia 2017 to 2021
Note:  : Male;
: Male;  : Female
: Female
Discussion
This study showed that majority of the TB cases are pulmonary as compared to extra-pulmonary and most of the cases were male (Table 1). Of the total cases on treatment, only few completed treatment during the period while majority were cured. A significant number of TB cases had HIV co-infection and a few of these were cured while the mortality rate among those with co-infection was 4% (Table 2).
| Description | Pulmonary TB (n=3349) | Extrapulmonary TB (n=760) | Total cases (n=4109) |
|---|---|---|---|
| Age group (in years) | |||
| 0-4 | 182 | 53 | 235 |
| 5-14 | 339 | 81 | 420 |
| >15 | 2828 | 626 | 3454 |
| Gender | |||
| Male | 1999 | 464 | 2463 |
| Female | 1350 | 296 | 1646 |
| Year | |||
| 2017 | 736 | 143 | 879 |
| 2018 | 690 | 136 | 826 |
| 2019 | 782 | 141 | 923 |
| 2020 | 670 | 167 | 837 |
| 2021 | 489 | 155 | 644 |
| Regions | |||
| Central River Region (CRR) | 74 | 22 | 96 |
| Lower River Region (LRR) | 72 | 19 | 91 |
| North Bank East Region (NBER) | 135 | 28 | 163 |
| North Bank West Region (NBWR) | 86 | 18 | 104 |
| Upper River Region (URR) | 259 | 37 | 296 |
| Western Region 1 (WR1) | 1647 | 452 | 2099 |
| Western Region 2 (WR2) | 1074 | 186 | 1260 |
Table 1: Proportion of TB cases (pulmonary and extrapulmonary) by demographic and geographic distribution in Gambia 2017-2021
| Treatment outcomes | ||
|---|---|---|
| Extrapulmonary TB (EPTB) | n=531 | % |
| Cured | 13 | 2.4 |
| Complete treatment | 460 | 86.6 |
| Died | 33 | 6.2 |
| Lost to follow | 21 | 4 |
| Failure | 1 | 0.2 |
| Not evaluated | 3 | 0.6 |
| Pulmonary TB (PTB) | n=5465 | % |
| Cured | 4714 | 86.3 |
| Complete treatment | 115 | 2.1 |
| Died | 274 | 5 |
| Lost to follow | 288 | 5.3 |
| Failure | 45 | 0.8 |
| Not evaluated | 26 | 0.5 |
Table 2: TB treatment outcomes in Gambia 2017-2021
This study showed that majority of reported TB cases in the country was pulmonary TB. A significant number of cases were under five years of age which is a cause for concern. Males constituted more than half of all cases. The cure and treatment completion rate were impressive with pulmonary TB cases had the highest cure rate with males accounted for the majority of deaths especially in pulmonary TB cases and this is similar to a study conducted in Zimbabwe in 2019, extrapulmonary TB have a high number that completed treatment, this is similar with a study conducted in Uganda in 2021. Most of the cases with co-infections are either on ARVs or CPT and many of these cases with co-infections recovered or are treated of TB (Table 3). Not-withstanding, some of these cases are lost to follow up and their outcome remains unknown if they are unreachable. The main limitation of the study was the fact that the predictors for treatment success could not be determined due to the unavailability of patient level data. The findings of limitation are similar to a study conducted in Uganda in 2021.
| TB-HIV co-infections (n=3572) | HIV-positive TB patients on ART | HIV-positive TB patients on CPT | HIV-positive TB patients cured | HIV-positive TB patients died | HIV-positive TB patients loss to follow | HIV-positive TB patients treatment completed | HIV-positive TB patients treatment failure |
|---|---|---|---|---|---|---|---|
| Male | 614 | 613 | 177 | 65 | 15 | 208 | 3 |
| Female | 676 | 702 | 176 | 79 | 11 | 228 | 5 |
Table 3: HIV positive-TB co-infection and outcomes in Gambia 2017-2021
Conclusion
Notification and documentation of the outcomes of treatment was never done during the period and this was as a result of the limited reporting indicators in the DHIS2. HIV positive TB cases had very low treatment failure within the five-year period.
In conclusion, there was high proportion of TB cases that completed their treatment and got cured. Though mortality was low, it was higher among pulmonary TB cases compared to extrapulmonary TB cases. This study also showed that co-infection with HIV was higher among females.
Ethical Approval and Consent to Participate
Ethical clearance has been given for the study and all participants and authors have given both verbal and written consent to participate in the study.
Consent for Publication
Consent has been given for the study to be published.
Availability of Data and Materials
The raw data generated for the analysis is available
Authors Contribution
Balla Jatta-Corresponding author, data collection, analysis, interpretation, writing; Peter Adewuyi-Helped in edition and review for content; Patrick Nguka-Helped in edition and review for content and mentoring; UC David-Helped in edition and review for content and concept development; Amadou Woury Jallow-Helped in data extraction and analysis; Sana Malang Sambou-Helped in data analysis and interpretation; Baba Kunta Fofana-Helped in edition; Mustapha Bittaye-Helped in edition and review for content; Wandifa Samateh-Helped in data extraction and analysis; Kebba
D. Sanneh-Helped in data extraction and analysis.
References
- Baluku JB, Nanyonjo R, Ayo J, Obwalatum JE, Nakaweesi J, Senyimba C, et al. Trends of notification rates and treatment outcomes of tuberculosis cases with and without HIV co-infection in eight rural districts of Uganda (2015-2019). BMC Public Health. 2022; 22(1): 651.
[Crossref] [Google scholar] [Pubmed]
- Teferi MY, El-Khatib Z, Boltena MT, Andualem AT, Asamoah BO, Biru M, et al. Tuberculosis treatment outcome and predictors in Africa: A systematic review and meta-analysis. Int J Environ Res Public Health. 2021; 18(20): 10678.
[Crossref] [Google scholar] [Pubmed]
- Harper M, Ahmadu FA, Ogden JA, McAdam KP, Lienhardt C. Identifying the determinants of tuberculosis control in resource-poor countries: Insights from a qualitative study in the Gambia. Trans R Soc Trop Med Hyg. 2003; 97(5): 506-510. PMID: 15307411.
[Crossref] [Google scholar] [Pubmed]
- Tesfahuneygn G, Medhin G, Legesse M. Adherence to anti-tuberculosis treatment and treatment outcomes among tuberculosis patients in Alamata district, northeast Ethiopia. BMC Res Notes. 2015; 8: 1-1.
[Crossref] [Google scholar] [Pubmed]
- Trends of notification rates and treatment outcomes of tuberculosis cases with and without HIV co-infection in eight rural districts of Uganda (2015-2019)
- Crossref
- National TB prevalence surveys. World health organization (WHO). 2021.
- Demographic and health survey. DHS program. 2021.
Author Info
Jatta Balla1*, Jallow Amadou Woury1, Sambou Sana Malang2, Adewuyi Peter3, Fofana Baba Kunta1,3, Nguka Patrick4, Umeokonkwo Chukwuma David4, Samateh Wandifa5, Sanneh Kebba D5 and Bittaye Mustapha62Department of Disease Control and Elimination, Medical Research Council, Banjul, Gambia
3Edward Francis Small Teaching Hospital, Ministry of Health and Social Welfare, Banjul, Gambia
4Department of Epidemiology and Disease Control, African Field Epidemiology Network, Kampala, Gambia
5Department of Infectious Diseases, National Leprosy and Tuberculosis Control Programme, Banjul, Gambia
6Department of Gynaecology, Ministry of Health, Banjul, Gambia
Citation: Balla J: Analysis of Tuberculosis Trends and Treatment Outcomes Data in Gambia Reported in the DHIS2 from 2017 to 2021
Received: 20-Jan-2023 Accepted: 03-Feb-2023 Published: 10-Feb-2023, DOI: 10.31858/0975-8453.14.2.122-124
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3