Research Article - (2022) Volume 13, Issue 10
Abstract
Novel Coronavirus Disease of 2019 or COVID-19 has striked the world again with an even more intense second wave. The association of poor mental health found with COVID-19 has been advocated by various resources. But very few studies have been done on the actual infected population. This research was carried out in the Psychiatry Department, Civil Hospital Sector 6, Panchkula, Haryana to find the prevalence of depression and anxiety among the COVID-19 positive patients. COVID-19 positive patients (n=4120) were telephonically called for mental health screening to look for the manifestation of either depressive behavior or anxiety using Personal Health Questionnaire- 9 (PHQ-9) and General Anxiety Disorder-7 (GAD-7) (respectively). The results showed the prevalence of anxiety (1.06%) among the infected population to be higher than current prevalence rate (0.57%) among the general Indian population for Generalized Anxiety Disorder but lower rate of depression (1.35%) as compared to the prevalence rate among the general population (2.7%). The study supports the direct impact of COVID-19 on the mental health of the infected patients.
Keywords
Depression, Anxiety, Coronavirus Disease (COVID-19), Severe Acute Respiratory Syndrome Corona Virus-2 (SARS-CoV-2)
Introduction
In late December 2019, the first-ever case of a never before seen virus was reported in Wuhan, China. This virus attacks its host in different manners, some of which are in the form of bronchial fibrosis, pyrexia and bodyache, weakness, loss of smell and taste, etc. (Utku AC, et al., 2020). Till date (10th May, 2021) over 239,200,000 cases have been reported with over 3,200,000 deaths all over the world (WHO, 2021). As a consequence of a global health crisis, drastic and strict measures by the public health administrations have been taken to tackle the novel Coronavirus SARS‐CoV‐2 (Coronavirus disease 2019; previously 2019‐nCoV) (Adhikari SP, et al., 2020). Despite these stringent control measures, the virus’ impact on India has been adverse especially after the second wave, making India the second country with the most positive cases in the world after USA.
Physiological manifestations aside, recently emerging researches are giving out straight evidence on the prevalence of psychological impact such as distress due to COVID-19 but most of these primarily focus on the general population rather than the infected population. A cross-sectional research in India indicated the prevalence of distress experienced by the general population during the pandemic (Anand V, et al., 2021). Another cross-sectional research from West Bengal showed that worry and sleep disturbances was common among the respondents (Chakraborty K and Chatterjee M, 2020). Studies have also shown the existing behavioral abnormalities developing in the frontline workers as a result of rampant spread of the virus (Cai Q, et al., 2020). In fact, the vice versa, i.e., the increased vulnerability to COVID-19 infection due to pre-existing mental illnesses has also been reported (Menon V and Padhy SK, 2020). While these researches provide hard evidence for the proliferation of psychological ailments associated with the emergence and widespread of SARS-CoV-2, they still cannot provide quantifiable data for psychopathological behavior exhibition as a result of presence of the disease in the body.
Due to the paucity of empirical research on the actually infected population that ensures psychological manifestation of the disease, it is wrong to conclude that the virus itself is responsible for the occurrence of psychological ailments. These ailments however could have been due to numerous factors like environmental, socio-economical, biological, etc. To comprehend the obscurity revolving around the theory of the virus itself being responsible for the development of psychopathological behavior, it is the need of the hour to study the existence of such behavior in the infected population. The most common psychological comorbidities that can be found in patients are depression and anxiety (Sartorius N, et al., 1996), so it was best to explore and examine these two to further gain insight into the impact of the virus on mental health.
This study was initiated with an aim to screen, identify and treat mental health issues in COVID-19 positive population remotely using the mechanism of tele-counseling (via audio and video calling) as it was infeasible to address their psychopathological issues via physical (offline) intervention. The screening was done with the hospital’s staff team consisting of trained professionals under supervision of a clinical psychologist. Screening involved interviewing to assess the patients for depression and anxiety symptoms, those screened in with scores showing anomaly were recommended for tele-counseling by the clinical psychologist. Patients whose scores came out as normal were asked if they wanted a ventilation session. Those who agreed were scheduled accordingly. The data was collected from all the patients consensually.
Methodology
The study employed a cross-sectional interview of COVID-19 positive people, whose contact details were arranged by the hospital authorities. This interview took place via audio calling. In order
Data collection
In view of the purpose of this study, the research depended mainly on primary data as the source of data collection.
• Primary data was obtained through calling individuals enlisted as the COVID-19 positive patient which was provided by the hospital as a part of a tele-counseling project initiated by the Psychiatry Department, Civil Hospital Panchkula.
• Secondary data was gathered by assessing two sources, first was the list provided by the COVID-19 testing department of the Civil Hospital for positive patients and the second source was various kinds of journals, online articles, etc., and over the topics related to the study.
Sampling
A total of 5000 samples were first interviewed, out of which 880 were discarded due to unavailability, wrong number, unanswered calls, COVID negative patients, preexisting mental disorders and if they were either family or friends of the patient. The age and gender was defined but was not taken in consideration for the purpose of research. This is because the sampling method used was purposive sampling method (Alvi M, 2016) for which the characteristic shared by the cohort was that the individual should be diagnosed with a COVID-19 positive test. The patients were informed about the intention of the calling and were provided an option to not to participate in the assessments. Intervention from interviewers’ side was strictly prohibited to ensure a completely voluntary participation by the patient. The patients were ensured confidentiality for responses as the recorded data is strictly stored under researchers’ supervision. In order to maintain the ethical integrity of these research necessary measures were given utmost priority and a strong sense of benevolence, non-maleficence, human dignity and legality was maintained. As the interview was taken verbally, chances for the risk of response duplication and biases were minimized. Names and contact details of the patients were deleted to avoid any breach of personal information of the patients to any third party. The patients whose scores showed signs of morbidity were also given an option to attend treatment sessions. Those who agreed were informed of the arrangements in accordance with both the patient and the psychologist. The paper has gone through the highly scrutinized and abiding process of approval for publication by the Scientific Research Committee (SRC) of the Civil Hospital, Panchkula.
Measurements
Study history: As the general information was already provided by the testing faculty from the hospital, most of the initial interview included collecting information on the current physiological statistics and past physiological as well as psychological morbidities. The later part included the assessments and referring the patient (if required) to the clinical psychologist.
Assessments
Personal Health Questionnaire-9 (PHQ-9): In order to test for the manifestation of depressive behavior, a 9 item scale popularly known as PHQ-9 was used as the first assessment. Personal Health Questionnaire-9 or PHQ- 9 is a self-reported questionnaire (Kroenke K, et al., 2001) that evaluates the presence of depressive symptoms during a specific time period of 2 weeks. Each item can be measured from 0 (not at all) meaning least observed during the period of 2 weeks to 3 (nearly every day) meaning most frequently observed during the same. The scoring is based on the severity of the symptoms and ranges from 0 to 27 for a total of 9 items. Scores falling in the range of 0-4 denotes No or negligible symptoms of depression, 5-9 denotes mild depression, 10-14 denotes moderate depression, 15-19 shows moderately severe signs for depression and 20 or above denotes severe signs for depression. The 9th item on the assessment questions if the respondent had experienced suicidal thoughts. To be quoted, it asks, “Thoughts that you would be better off dead, or thoughts of hurting yourself in some way?” If the respondent’s score falls in the normal range but has scored even a single point in item number 9, the overall diagnosis tips into the direction of depressed behavior.
Telephonic administration of PHQ-9 for depression yields similar results (Pinto-Meza A, et al., 2005) as the ones that are self-administered in the physical world, eliminating scopes for inaccurate outcomes.
General Anxiety Disorder-7 (GAD-7): In order to observe the symptoms for general anxiety, a 7 item scale popularly known as GAD-7 was used as the second assessment. General Anxiety Disorder-7 or GAD-7 is also a self-reported questionnaire (Spitzer RL, et al., 2006) that evaluates the presence of depressive symptoms during a specific time period of 2 weeks. Each item can be measured from 0 (not at all) meaning least observed during the period of 2 weeks to 3 (nearly every day) meaning most frequently observed during the same. The scoring is based on the severity of the symptoms and ranges from 0 to 21 for a total of 7 items. Scores falling in the range of 0-4 denotes No or negligible symptoms of anxiety, 5-9 denotes mild anxiety, 10-14 denotes moderate anxiety and scores equal to or more than 15 implies severe anxiety.
The instruments were used exclusively for the purpose of research and assessing the patients as they suited the best given that the average isolation period recommended was for about 2 weeks. Both the assessment tools inquire about the frequency of such behavior observed within a period of 2 weeks as well. The psychometric properties of both PHQ-9 (Gilbody S, et al., 2007) and GAD-7 (Johnson SU, et al., 2019) have been tested and verified in past studies.
Data analysis
The data analysis was carried out using a descriptive model on Jamovi, a statistical spreadsheet analysis tool. The data was entered and as for the descriptive of raw-unevaluated scores, mean, median, standard deviation and maximum scores were evaluated. The scores were then manually evaluated to be further sorted into corresponding severity categories relevant to each of the assessment tools used. Descriptive statistical methods were used to summarize data on the number of patients who had experienced symptoms for depression and anxiety (Team RC, 2020). Tables were developed using the Frequency Tables tool in Jamovi, whereas the Figures were developed using Google Spreadsheet for the same data.
Results
Out of the 4120 patients, a total of 2.4% (n=99) came out to have manifested psychological disturbances that developed after being infected by SARS-CoV-2. For depression, on the scale of PHQ-9 (Table 1 and Figure 1), 98.64% (n=4064) of the cohort depicted no or minute symptoms as their scores ranged in the normal category. Patients who showed symptoms for depressed mood were 1.35% (n=56) out of which 0.73% (n=30) were mildly depressed, 0.56% (n=23) were moderately depressed and 0.05% (n=2) came to be in the moderately severe category. Only a fraction of the sample, i.e 0.02% (n=1) of the patients came in the range of severely depressed implying with a score equal to or more than 20.
| Levels | Counts | % of total | Cumulative% |
|---|---|---|---|
| Normal | 4064 | 98.64 % | 98.60% |
| Mild | 30 | 0.73 % | 99.40% |
| Moderate | 23 | 0.56 % | 99.90% |
| Moderately severe | 2 | 0.05 % | 100% |
| Severe | 1 | 0.02 % | 100% |
Table 1: Personal Health Questionnaire-9 (PHQ-9) Outcomes
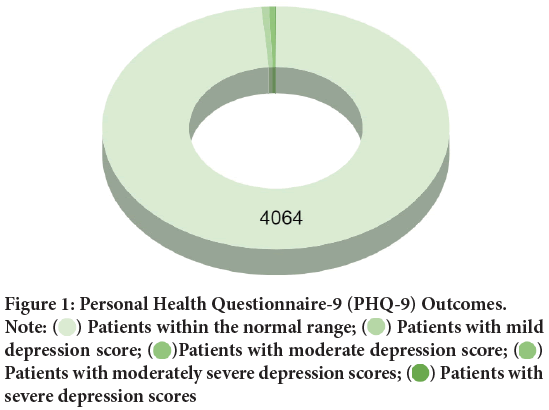
Figure 1: Personal Health Questionnaire-9 (PHQ-9) Outcomes. Note:  Patients within the normal range;
Patients within the normal range;  Patients with mild
depression score;
Patients with mild
depression score;  Patients with moderate depression score;
Patients with moderate depression score;  Patients with moderately severe depression scores;
Patients with moderately severe depression scores;  Patients with
severe depression scores
Patients with
severe depression scores
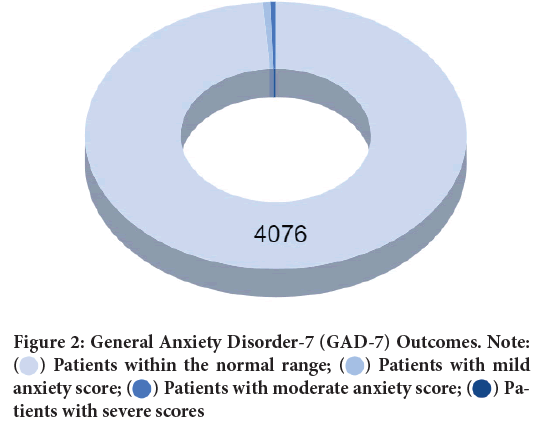
For GAD-7 (Table 2 and Figure 2) which was used to assess symptoms for anxiety on the same population, a significant sum of sample constituting up to 98.93% (n=4076) fell in the range of normal category. 1.06% (n=44) of the patients faced symptoms of anxiety as 0.63% (n=26) of the total sample had scores in the range of mild anxiety, 0.41% (n=17) had scores in moderate anxiety and 0.02% (n=1) had scores falling into the range of severe anxiety. There was only 0.02% (n=1) of the sample that overlapped and showed symptoms for depression and anxiety, rest of the results were all mutually exclusive.
| Levels | Counts | % of total | Cumulative% |
|---|---|---|---|
| Normal | 4076 | 98.93 % | 98.9% |
| Mild | 26 | 0.63 % | 99.6% |
| Moderate | 17 | 0.41 % | 100% |
| Severe | 1 | 0.02 % | 100% |
Table 2: General Anxiety Disorder-7 (GAD-7) Outcomes
Figure 2: General Anxiety Disorder-7 (GAD-7) Outcomes. Note:  Patients within the normal range;
Patients within the normal range;  Patients with mild
anxiety score;
Patients with mild
anxiety score;  Patients with moderate anxiety score;
Patients with moderate anxiety score;  Patients with severe scores
Patients with severe scores
As for the descriptive of the scores (Table 3), for PHQ-9 the mean score was 0.980 out of 27, median was 0, the standard deviation (σ) came out to be 1.50 and the maximum score recorded was 20. As for GAD-7, the mean score came out to be 0.665, the median was 0, standard deviation (σ) was 1.34 and the maximum score recorded was 15. Minimum scores recorded for both PHQ-9 and GAD-7 were both 0.
| Descriptive | PHQ-9 | GAD-7 |
|---|---|---|
| N | 4120 | 4120 |
| Mean | 0.98 | 0.665 |
| Median | 0 | 0 |
| Standard deviation | 1.5 | 1.34 |
| Minimum | 0 | 0 |
| Maximum | 20 | 15 |
Table 3: Comparative descriptive for Personal Health Questionnaire-9 (PHQ-9) and General Anxiety Disorder-7 (GAD-7)
Discussion
This study aimed at determining whether the existence of direct impact on the psychological health caused by Coronavirus is actually there or not. The results came out inconsistent for depressive symptomatology but consistent for the prevalence of general anxiety disorder as claimed by numerous studies and articles out there as according to them, it can be inferred that the prevalence of symptoms for depression and anxiety acts as a potential risk/predisposing factor among the infected population. To comprehend the results, it would be appropriate to compare the current prevailing rate of depression and anxiety among the general population with that of COVID-19 positive sample population. According to the National Mental Health Survey 2015-2016 report by National Institute of Mental Health and Neurosciences (NIMHANS, Bengaluru), the current prevalence rate of depressive disorders among the general Indian population is 2.7. Also, the rate of prevalence of general anxiety disorder or GAD is 0.57 (Murthy RS, 2017).
For the signs of depressed behavior, the results evaluated using PHQ-9 depict that prevalence of depression was 1.35% among the infected study population which is lower than that found among the general population as per the report by NIMHANS. There was only one patient who had suicide ideation and it was the same person with highest PHQ-9 score which was 20. Most of the patients with depressed mood came out to be mildly depressed with 0.73% of the total sample or say 53.57% of the psychologically depressed population. 0.56% of the total sample felt moderately depressed after contacting the virus, which makes 41.07% of the psychologically depressed sample. 0.05% and 0.02% of the total infected sample fell in the category of moderately severe and severely depressed respectively which makes 3.57% and 1.79% of the depressed population. The percentage of people that came out to be normal when assessed for depressive behavior was 98.64% which suggests that Coronavirus of 2019 is not directly responsible for manifestation of depressive mood.
Coming to the aspects of developing anxiety as a direct impact of said virus, the results for GAD-7 assessments vary far from the results evaluated using PHQ-9. Out of 4120 screened sample, 1.06% scored out of the normal range when compared to current prevailing rate of GAD which is 0.57% providing evidence for the direct role of COVID-19 in developing anxious behavior among the infected population. 0.63% was mildly affected which is 59.09% of those showing symptoms for anxiety. The patients with moderate and severe anxiety were 0.41% and 0.02% respectively of the total population. These summed up to be the 38.64% and 2.27% of patients with anxiety. Sample that showed no symptoms for anxiety was a percentage of 98.93% which could seem to be misleadingly concealing the prevalence of anxiety among the patients infected with Coronavirus. It is in fact almost double the current rate among the general population.
The average scores for both PHQ-9 and GAD-7 came in the normal range. The mean score for PHQ-9 was 0.980 and for GAD-7 it was 0.665. As many of the patients scored 0 for both the assessments, the median came out as 0. On an average, the scores varied as far as 1.50 for PHQ-9 and 1.34 for GAD-7 as depicted by standard deviation (σ) for both the assessments. The maximum score registered for PHQ-9 was 20 on a scale of 0-27 whereas on a scale of 0-21, it was 15 for GAD-7. These maximum scores were registered once for both the assessments. These indicate that on an average being COVID-19 positive does not qualify as a predisposing factor or plays a direct role in influencing an individual’s psychopathology abnormally. While the whopping percentage of patients with normal range in both the assessments mirages the situation of existing psychopathological risks as a non-threatening position, the contrastingly alarming results for GAD-7 clearly provides the evidence of psychological disturbances faced by the cohort. In fact the results for PHQ-9 although may be less intimidating but shall not be neglected as a potential endangerment to the psychological health of the infected population (Panchal N, et al., 2020).
The study after testing accepts the existence of anxiety among the COVID-19 positive population but on the other hand, raises questions for its manifestation inducing depressive behavior. Providing pragmatic and cogent implications in taking preventive stratagem safeguarding the mental health of the infected population, this research could help form the basis to layout requisite amendments in the public health administration strategies during a pandemic. It suggests that the directly affected population is at high risk for developing depressive psychopathology while providing solid evidence for their vulnerability to developing anxiety. To prevent such distressing developments timely non-pharmacological treatments (largely the psychosocial interventions) could be appropriately delivered. Although some of such interventions have already been initiated by the State and Central Government of India like toll free helplines and tele counseling services for mental health assistance, nevertheless the implications have not yet been enforced at par with the adversity of the situation.
It is also evident that COVID-19 does not directly play a role in increased depression rates but it is rather the psycho-social dynamics that have fabricated an unstable scenario for the citizens as a consequence of protocols implied to tackle the outspread. This implies an evident indirect impact that the virus has made onto the mental health of a big chunk of society. To address the prevalence of anxiety among the infected population which is admitted in the hospitals, a team of mental health professionals should be formulated with adequate resources such as equipment and hazmat suits enabling them to enter isolation wards aiding in identification as well as the intervention of anxiety issues. Another issue which was raised by numerous patients that sourced their anxieties and apprehensions were their worries for recovering from the disease. The public administration can provide reassurance regarding the same by mapping out a system of following up with the patients for an example via Ecological Momentary Assessments and opening of Post-COVID clinics like UMANG as done by the State Medical Administration of Panchkula which provides a platform for rehabilitation/monitoring of adversely affected population. Depressive vulnerability although has come out low in this research but the figures were almost closing in with the prevalent contemporary rate among the general population, many respondents raised the topic of lack of socio-economic stability being the reason of their distress while interviewing the patients. Lack of financial resources in a pandemic with so many stringent restrictions has made it difficult for the middle and lower class families to cope up with the overwhelming stress that has come along with the virus outbreak. Certain policies to help the Economically Weaker Section or EWS should also be constituted.
Conclusion
Unequivocally, in these distressful times of epidemiological crisis no one feels safe and many are deprived of even the basic standards of being ‘healthy.’ People have been robbed of their physical, mental and most importantly their social well-being. Especially the ones infected with the virus are secluded from the rest of the world and confined within a limited space alone with constant uncertainty and distress about their physical well-being that tags along with dire health. Evident as it has been, the mental impact of such a crisis outlasts the physical impact and desperately requires it to be addressed timely. While the public administration holds the helm to make extensive reforms, even the minute efforts contributed at individual level will also assist in constraining the outbreak of the virus. With this study, it is suggested to take collective measures that include the perspectives of various stakeholders in order to deal with the pandemic of COVID-19 with much more resilience, resourcefulness, pragmatism and efficacy.
Limitations
This study will be one of the first studies conducted directly on the COVID-19 infected population and would significantly add to the literature of mental health and Coronavirus. But that does not imply that this one has no limitations. One scope of improvisation is to include more population specific variables like age, gender and socio-economic status which were excluded due to issues with patient confidentiality. Also, the fact that the study was conducted during a 14-17 day incubation period of COVID-19 symptoms which could have played a role in deterioration of the patients’ mental health. It is suggested for future researchers to conduct this study during the incubation period as well as post treatment to check if the results differ in any sense.
References
- Utku AC, Budak G, Karabay O, Güçlü E, Okan HD, Vatan A. Main symptoms in patients presenting in the COVID-19 period. Scott Med J. 2020; 65(4): 127-132.
[Crossref] [Google Scholar] [Pubmed]
- WHO. Coronavirus disease (COVID-19) situation reports. World Health Organization. 2021.
- Adhikari SP, Meng S, Wu YJ, Mao YP, Ye RX, Wang QZ, et al. Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of Coronavirus disease (COVID-19) during the early outbreak period: A scoping review. Infect Dis Poverty. 2020; 9(1): 1-2.
[Crossref] [Google Scholar] [Pubmed]
- Anand V, Verma L, Aggarwal A, Nanjundappa P, Rai H. COVID-19 and psychological distress: Lessons for India. Plos One. 2021; 16(8): 255683.
[Crossref] [Google Scholar] [Pubmed]
- Chakraborty K, Chatterjee M. Psychological impact of COVID-19 pandemic on general population in West Bengal: A cross-sectional study. Indian J Psychiatry. 2020; 62(3): 266.
[Crossref] [Google Scholar] [Pubmed]
- Cai Q, Feng H, Huang J, Wang M, Wang Q, Lu X, et al. The mental health of frontline and non-frontline medical workers during the Coronavirus disease 2019 (COVID-19) outbreak in China: A case-control study. J Affect Disord. 2020; 275: 210-215.
[Crossref] [Google Scholar] [Pubmed]
- Menon V, Padhy SK. Mental health among COVID-19 survivors: Are we overlooking the biological links?. Asian J Psychiatr. 2020; 53: 102217.
[Crossref] [Google Scholar] [Pubmed]
- Sartorius N, Üstün TB, Lecrubier Y, Wittchen HU. Depression comorbid with anxiety: Results from the WHO study on psychological disorders in primary health care. The Br J Psychiatry. 1996; 168(S30): 38-43.
[Crossref] [Google Scholar] [Pubmed]
- Alvi M. A manual for selecting sampling techniques in research. Munich Personal RePEc Archive. 2016.
- Kroenke K, Spitzer RL, Williams JB. The PHQ‐9: Validity of a brief depression severity measure. J Gen Intern Med. 2001; 16(9): 606-613.
[Crossref] [Google Scholar] [Pubmed]
- Pinto‐Meza A, Serrano‐Blanco A, Penarrubia MT, Blanco E, Haro JM. Assessing depression in primary care with the PHQ‐9: Can it be carried out over the telephone?. J Gen Intern Med. 2005; 20(8): 738-742.
[Crossref] [Google Scholar] [Pubmed]
- Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch Intern Med. 2006; 166(10): 1092-1097.
[Crossref] [Google Scholar] [Pubmed]
- Gilbody S, Richards D, Brealey S, Hewitt C. Screening for depression in medical settings with the Patient Health Questionnaire (PHQ): A diagnostic meta-analysis. J Gen Intern Med. 2007; 22(11): 1596-1602.
[Crossref] [Google Scholar] [Pubmed]
- Johnson SU, Ulvenes PG, Øktedalen T, Hoffart A. Psychometric properties of the General Anxiety Disorder 7-item (GAD-7) scale in a heterogeneous psychiatric sample. Front Psychol. 2019; 10: 1713.
[Crossref] [Google Scholar] [Pubmed]
- Team RC. R: A language and environment for statistical computing. The Comprehensive R Archive Network. 2020.
- Murthy RS. National mental health survey of India 2015-2016. Indian J Psychiatry. 2017; 59(1): 21.
[Crossref] [Google Scholar] [Pubmed]
- Panchal N, Kamal R, Orgera K, Cox C, Garfield R, Hamel L, et al. The implications of COVID-19 for mental health and substance use. Kaiser family foundation. 2020; 21.
Author Info
Anu Bansal, Karan Samdhian*, Veena Sharma, Ankita Chaudhary, Mahendra Prakash Sharma and Manoj KumarCitation: Bansal A: Descriptive Analysis Exploring the Prevalence of Depression and Anxiety as a Direct Impact of COVID-19 on Infected Population
Received: 15-Sep-2022 Accepted: 10-Oct-2022 Published: 17-Oct-2022, DOI: 10.31858/0975-8453.13.10.722-726
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3