Research Article - (2021) Volume 12, Issue 11
Effects of All-Trans-Retinoic Acid on Over Cancer Culture (Ovcar-3) Alone and Combined with Classical Chemotherapeutics
Hulusi Goktug Gurer1, Ceren Yildiz Eren1*, Ozlem Ozgür Gursoy1, Ayşe Tansu Koparal2 and Sabit Sinan Ozalp3Abstract
Background: Ovarian cancer is the most common cause of gynecological cancer deaths; it has a very important place in gynecological oncology. Combination therapy is a treatment method that combines more than one agent used in treatment. Today it is one of the most important weapons in cancer treatment. In this study, the aim was to examine the sole and combined effects of classical CT drugs and ATRA on Ovcar-3 cells in vitro.
Methods: To determine the effects of carboplatin, paclitaxel, and ATRA on Ovcar-3 cells, MTT, DAPI staining, caspase-3 and real-time PCR analyses was performed.
Results: It was observed that the combination of paclitaxel+carboplatin+ATRA significantly decreased cell viability at all doses on all days. DAPI staining showed apoptosis. In apoptotic cells, it was observed that the nuclei strangulated, divided into small pieces, and condensed. Among the combinations, the highest increase in caspase-3 activity was recorded with the combination of ATRA+paclitaxel. It was observed that combined applications do not have a reduction effect on gene activations as much as single applications.
Conclusions: In this study, ATRA and other agents sole and in combination showed significant anticancer effects in MTT, DAPI Staining and Caspase-3 analyses in Ovcar-3 cancer cell lines. In Real-Time PCR analysis, ATRA and other agents showed similar anticancer effects when applied alone. However, the same effect was not observed when agents combined and this is different from some results in the literature. Researching this subject with new studies will contribute to the literature.
Keywords
ATRA, Cancer therapy, mbination therapy, Ovcar-3 cell lines
Introduction
Cancer is a disease that claims the lives of approximately ten million people a year worldwide. The biggest challenge we face in cancer treatment today is the lack of anticancer drugs with high efficacy, broad-spectrum and low side effects. In this respect, innovative approaches in drug development are extremely important. In the light of advances in molecular biology, drug development studies against cancer have gained momentum all over the world, although the discovery and development of anticancer drugs are progressing slowly. It is aimed to create clinical paradigms around the world in anti-cancer drug development. Global participation and cooperation in this area is supported (Jauregui DL, et al., 2020).
Cancer is an important problem that has serious effects on the health system. Despite advances in diagnosis, prevention methods, and treatments, it still affects millions of people all over the world. Because ovarian cancer is the most common cause of gynecological cancer deaths, it has a very important place in gynecological oncology. Ovarian cancer is the fifth most common malignancy among cancers seen in women. It ranks fourth in cancer deaths in women. Every year, more than 295,000 new ovarian cancer diagnoses are made, and this type of cancer causes more than 184,000 deaths worldwide. In ovarian malignancies, which have an extremely important place in terms of general women's health, the main treatment is surgery and subsequent chemotherapy. cisplatin, carboplatin, cyclophosphamide, and paclitaxel are effective drugs alone against ovarian cancer. Among these drugs, the combination of platinum with taxanes is preferred (Visconti RM and Morea D, 2019; McMullen M, et al., 2021; Kumar BS, et al., 2018; Bray F, etal., 2018).
Cell culture is a versatile system frequently used in scientific research. Its advantage is uniformity and repeatability. Cell culture includes methods that allow prokaryotic and eukaryotic cells to develop under physiological conditions. Cell culture is most commonly used for examining cell biology, researching disease mechanisms, and drug research. Cell culture is used to examine the metabolism and toxicity of drugs developed due to ethical and economic concerns. Cell culture is considered to be the most reliable method in drug studies and in vitro research. In addition, studies on the interaction of drugs with each other are also carried out in cell culture (Jaroch K, et al., 2018; Segeritz CP and Vallier L, 2017).
Combination therapy is a treatment method that combines more than one agent used in treatment. Combination therapy is one of the most important weapons in cancer treatment today. Compared to the use of one agent alone, the use of more than one agent together increases the effectiveness of the treatment by showing a synergistic effect. Other benefits of this application are reduction in drug resistance and metastasis development. Combination therapy also has effects such as arresting the mitosis potential of cells and inducing apoptosis. Five-year survival is low for many types of cancer. The development of drugs to be used in this field is an economically demanding and less time-consuming process. For these reasons, a tendency has been made towards cost-effective, time-consuming, and prolonged survival practices. As a result of this orientation, combination therapies are preferred among today's cancer treatment approaches (Mokhtari RB, et al., 2017).
There are many studies conducted to find effective drugs in the treatment of ovarian cancers. Studies conducted for this purpose show that All-Trans-Retinoic Acid (ATRA), a natural retinoid, stops the growth of cancer cells. ATRA is a physiologically active metabolite of vitamin A. The Insulin Receptor Substrate-1 (IRS-1) factor is known to trigger proliferation in various tumor types. Some studies have shown that ATRA has a potential role in suppressing gynecological cancer cells. It was found that IRS-1 protein levels decreased by suppression in cells treated with ATRA (Costantini L, et al., 2020).
In this study, the aim was to examine the sole and combined effects of classical CT drugs (carboplatin and paclitaxel) and ATRA, a natural retinoid, on Ovcar-3 cells by applying in vitro tests. For this purpose, cytotoxic and apoptotic effects of combined therapy were examined. The examination was carried out with the Tetrazolium Test (MTT assay), which is based on the measurement of mitochondrial activity. Apoptotic effects were examined by DAPI staining and caspase-3 Elisa colorimetric kit test, which showed changes in nuclear DNA. In addition, the expression of IRS-1, Kinase Inhibitor-67 (Ki-67), Vascular Endothelial Growth Factor (VEGF), and Cyclooxygenase-2 (COX-2) genes were investigated by Real-Time PCR.
Materials and Methods
Preparation of materials
Glass and plastic materials and liquid solutions used in the studies were kept in an autoclave at 121°C for 20 minutes at 1.5 atm/Hg pressure, and at 180°C for 2 hours in a sterilizer. Some liquid chemicals used were passed through a 0.2 mm spaced cellulose nitrate filter.
Preparation of drug dosages
Drug doses were prepared by dissolving ATRA, paclitaxel, and carboplatin in DMSO (1:40 ratio). Doses were used as soon as they were prepared. The doses to be used were determined using the information obtained from literature reviews.
Cells
Ovcar-3 cells were purchased from American Type Culture Collection (ATCC). Ovcar-3 cells were grown in 20% Fetal Bovine Serum, penicillin-streptomycin, sodium bicarbonate, MEM Non-essential amino acid solution, RPMI 1640 medium at 37°C in a medium containing 5% CO2.
MTT assay
To determine the cytotoxic effects of carboplatin, paclitaxel, and ATRA on Ovcar-3 cells, MTT [3-(4,5-dimethythiazol-2-yl)-2,5-diphenyl tetrazolium bromide] analysis was performed. After determining the viability of the cells by Trypan Blue staining, the cells were counted with Thoma slide and cultured in 96-well plates at 5 × 104 cells per well for 24 hours. At the end of this process, the medium in the wells was emptied and the media containing different concentrations of test substances were placed in the plates. At the end of the incubation period, the media were removed from the treated cells for the periods determined by the test substances (24 hours, 24, and 48 hours, 72 hours). The cells were incubated with 5 mg/ml-1 MTT solution for two hours to convert the MTT dye to the water-insoluble formazan salt. At the end of this period, MTT dye was removed from the cells. 0.1 ml DMSO was added to each well to dissolve the formazan salts formed by living cells. Optical densities of the cells in the plates were read on an ELISA device (Spectra max 340 PC Molecular Devices, LLC USA) at a wavelength of 570 nm. The viability rates of the test cells are expressed as a percentage, assuming the control cell viability rate not treated with the test substance as 100%. Experiments in which cells were planted in parallel for each dose of test substance in experiment sets were repeated three times independently of each other. IC50 doses determined by applying the agents alone were used in combinations. SPSS program was used in the statistical evaluation of the results of MTT experiments and the significance levels of the obtained data were determined by applying one-way ANOVA and Tukey test as a post-hoc. The significance limit was determined as p<0.05.
Apoptosis assay
Morphological examination with fluorescent staining (DAPI staining): DAPI staining was performed to determine the apoptotic effects of carboplatin, paclitaxel, and ATRA doses determined as a result of the MTT assays on Ovcar-3 cells. Cells were seeded into six-well plates with sterile round lamellas and cultured in a 24 hour CO2 incubator. At the end of this period, the medium in the wells was removed. The effective doses of the agents determined as a result of the cytotoxicity tests were applied to the cells adhered on the lamellae for 12 hours. The medium was then removed from the wells, lamellas were washed with sterile phosphate buffer solution (PBS: 137 mM NaCl, 2.7 mM KCl, 15 mM KH2PO4, 8 mM NaHPO4 ; PH 7.3), detected for 15 minutes at 37°C in 3.7% paraformaldehyde solution dissolved in PBS. After detection, lamellas were washed 3 times with PBS and incubated for 30 minutes at 37°C with 1 mg/ml 4'6-Diamidino-2 Phenylindole (DAPI) in a dark environment. The lamellas were then washed with PBS and capped and photographed under a fluorescent microscope.
Caspase 3 analysis: The cells were dissected according to the method the company from which the caspase-3 kit was purchased to collect the cell contents and analysis was performed. As a result of the analysis, the plates were read with an Eliza microplate reader at a wavelength of 405 nm (R and D systems, Inc. 1-800-343-7475). In the statistical evaluation of the results, the SPSS program was used and the significance levels of the obtained data were determined by applying one-way ANOVA and post-hoc Tukey test. The significance limit was accepted as p<0.05.
Real-Time PCR
RNA isolation:Ovcar-3 cells were cultivated in 75 cm2 flasks as 1 × 104 cells and incubated for 48 hours. Following the incubation, cells were exposed to the specified concentrations of substances based on the data obtained from the results of the MTT assay. After the cells were treated with the substances for 24 hours, the cells were collected into the centrifuge tube with the help of PBS, PBS-EDTA, trypsin together with the supernatant. By using Thoma slide, 4 × 106 cells were taken and the supernatant was centrifuged at 1250 rpm for six minutes. Buffer RTL plus+Beta mercaptoethanol mixture was placed on the cells and placed in columns holding genomic DNA and centrifuged at 10,000 rpm for 1.5 minutes. In this way, genomic DNA has been ensured to remain in the column. 350 µl of 70% ethanol was added onto the lysate where the genomic DNA was not found below and it was centrifuged at 10,000 rpm for one minute by placing it in pink-colored columns. The underlying liquid was removed, 700 µl RW1 was added to the column, centrifuged at 10,000 rpm for 15 seconds and the liquid was removed. 500 µl Buffer RPE was placed on the pink columns and centrifuged at 14 000 rpm for one minute. Then the pink columns were placed on a new collection tube and the same process was repeated by centrifuging at 14 000 rpm for three minutes. The column was placed in a new collection tube to dry without adding anything, and centrifuged for one minute at 14 000 rpm. After the column was placed in a new clean Eppendorf tube, 40 μl RNAse Free Water was added on it and centrifuged at 10 000 rpm for 1.5 minutes. By throwing the upper column, the underlying RNAs were measured and stored at -80°C until the process was performed for real-time PCR. Real-time PCR analysis was performed on BioRad, Hercules, California, USA.
RNA concentration measurement: To determine the amount and purity of the RNA, the isolated RNA was measured in a nanodrop device, DNAse was diluted with RNAse free water.
cDNA sy nthesis: For cDNA synthesis, the reaction was prepared with a total volume of 20 μl and cDNA synthesis was performed on a palm cycler device.
Relative quantification:The concentration of the target is expressed as the ratio of the target to a certain reference. To determine the concentrations of target and reference genes, the use of standard curves of both is necessary when using this method. In our study, while interpreting our real-time PCR results, the concentration value of our target genes was proportioned to the concentration value of the reference gene, and how much the results obtained differed compared to the control group were examined. It is a "housekeeping" gene that is constantly expressed in all cells. The housekeeping gene encodes proteins involved in cell functioning and is therefore always expressed. The 18S rRNA gene is one of the frequently preferred internal control genes in Real Time-PCR studies related to cancer studies. In relative gene expression comparison studies, the best result is obtained by including the internal control in the sample. An unchanged endogenous control is used for the quantification of different target mRNAs in each reaction. The 18S rRNA gene was used for this purpose in our study (Kuchipudi SV, et al., 2012).
Results and Discussion
MTT assay results
Doses of ATRA in the range of 10-250 µM caused an increase in the number of cells in Ovcar-3 cells in the first 24 hours according to the control. Cell viability decreased at doses of 250 µM and 270 µM. Cell viability decreased statistically significantly at all doses after 48 hours. Cell viability increased at the dose of 10 µM at the end of 72 hours and decreased statistically significantly with increasing dose (Figure 1).
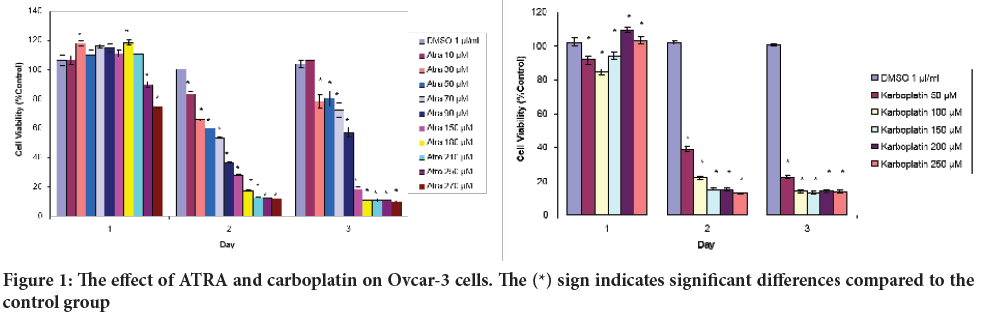
Figure 1: The effect of ATRA and carboplatin on Ovcar-3 cells. The (*) sign indicates significant differences compared to the control group
Cell viability increased at the end of 24 hours at 200 and 250 µM doses of carboplatin. On the second and third days, a significant decrease was observed in all doses.
It was observed that paclitaxel significantly decreased cell viability at all doses on the 1st, 2nd and 3rd days. It was determined that the decrease was more pronounced at doses of 5 µM and above on the second and third days (Figure 2).
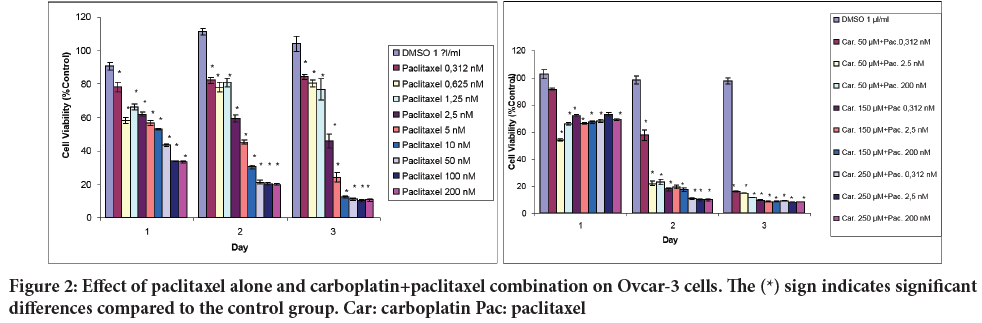
Figure 2: Effect of paclitaxel alone and carboplatin+paclitaxel combination on Ovcar-3 cells. The (*) sign indicates significant differences compared to the control group. Car: carboplatin Pac: paclitaxel
In the combination of carboplatin and paclitaxel, a statistically significant decrease in cell viability was noted on all days. While the decrease in cell viability was evident at low doses on the first day, an increase in viability was observed as the dose increased. The decrease is more pronounced on the second and third days and is directly proportional to the dose increase.
There was no significant decrease in the viability of cells in the first 24 hours with the combination of ATRA+paclitaxel according to the control group. When the cell viability was examined at the end of 48 and 72 hours, a significant decrease was observed. The reduction is likely to be significantly due to paclitaxel, as the decrease in viability of the cells compared to the control group was low at the low dose of paclitaxel, 0.312 µM. Cell viability was significantly reduced when the dose of paclitaxel was increased while the ATRA dose remained the same (Figure 3).
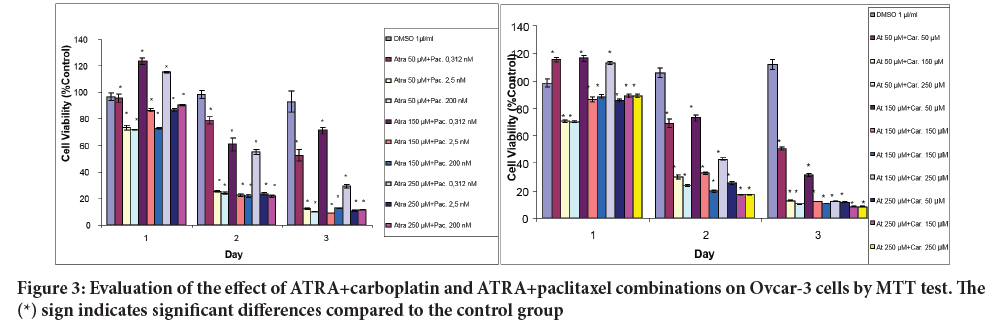
Figure 3: Evaluation of the effect of ATRA+carboplatin and ATRA+paclitaxel combinations on Ovcar-3 cells by MTT test. The (*) sign indicates significant differences compared to the control group
In the combination of ATRA+carboplatin, results parallel to the combination of ATRA+paclitaxel were obtained. There was no significant decrease in the viability of the cells in the first 24 hours according to the control group. Significant reduction in cell viability was observed at the end of 48 and 72 hours. It is likely that the decrease is significantly due to carboplatin. At the low dose of carboplatin, 50 µM, the decrease in the viability of cells was low according to the control group. Cell viability decreased significantly when the carboplatin dose was increased while the ATRA dose remained the same.
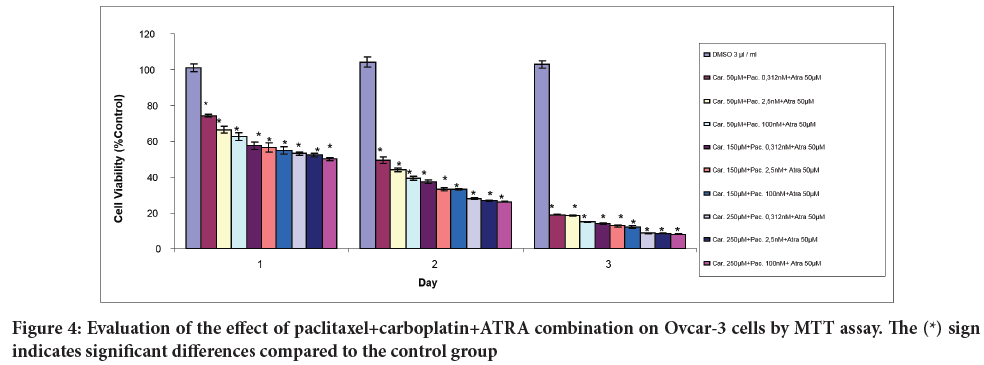
It was observed that the combination of paclitaxel+carboplatin+ATRA significantly decreased cell viability at all doses on the 1st, 2nd, and 3rd days (Figure 4).
Figure 4: Evaluation of the effect of paclitaxel+carboplatin+ATRA combination on Ovcar-3 cells by MTT assay. The (*) sign indicates significant differences compared to the control group
DAPI staining results
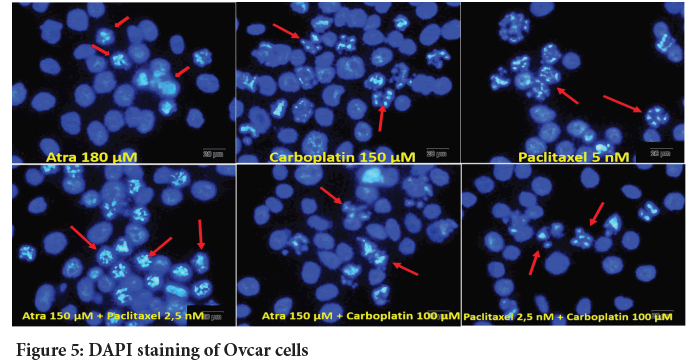
DAPI staining was performed to morphologically determine the apoptotic effects of ATRA, carboplatin and paclitaxel alone and in combination on Ovcar-3 cells. ATRA, carboplatin and paclitaxel, which were found to be effective as a result of MTT assays, were administered to the cells alone and in combined doses. The cells are then photographed. Arrows in the photographs show apoptotic cells. In apoptotic cells, it was observed that the nuclei strangulated, divided into small pieces, and condensed (Figure 5).
Figure 5: DAPI staining of Ovcar cells
Caspase-3 results
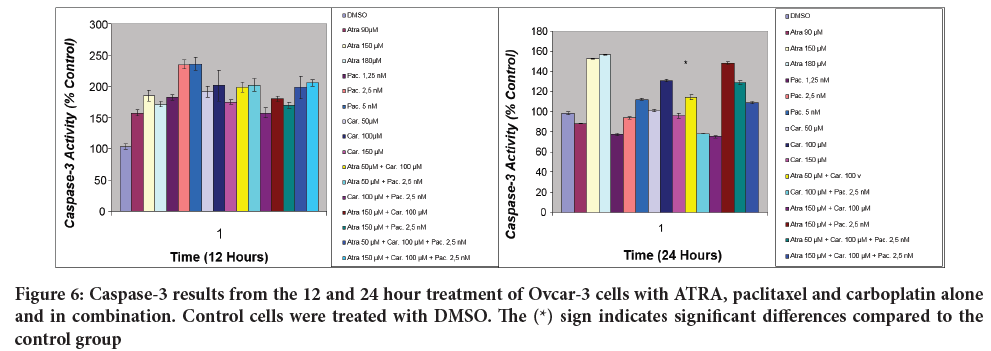
The effects of ATRA, paclitaxel and carboplatin on the caspase-3 activities of Ovcar-3 cells at the end of 12 and 24 hours are presented in Figure 6. At the end of 12 hours, all of the agents appear to increase caspase-3 activity in all doses administered alone or in combination. At the end of 12 hours, paclitaxel showed the most significant effect on caspase-3 activities at 2.5 and 5 nM doses. At the end of 24 hours, it was observed that the agents exhibited different effects at different doses. While the activity of caspase-3 decreased at 90 µM dose of ATRA, the activity increased more than other agents at 150 and 180 µM doses. paclitaxel and carboplatin doses of 5 nM and 100 µM, respectively, increased the caspase-3 activity more than other doses. Among the combinations, the highest increase in caspase-3 activity was recorded with the combination of ATRA 150 µM+paclitaxel 2.5 nM (Figure 6).
Figure 6: Caspase-3 results from the 12 and 24 hour treatment of Ovcar-3 cells with ATRA, paclitaxel and carboplatin alone and in combination. Control cells were treated with DMSO. The (*) sign indicates significant differences compared to the control group
Evaluation of Real-Time PCR results
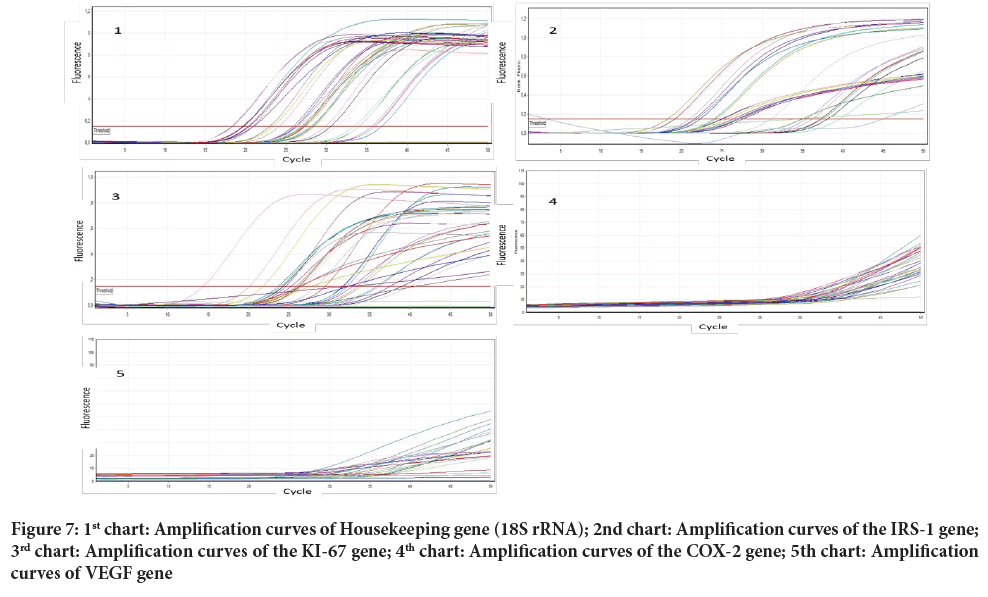
Ovcar-3 cells were treated for 24 hours with different doses and combinations of ATRA, paclitaxel and carboplatin. Substance and dose dependent activation states in the IRS, Ki-67, COX-2 and VEGF genes in the cell line after the treatment were tried to be determined by RT-PCR technique. According to the studies, 90, 150 and 250 µM ATRA doses administered alone caused a decrease in IRS and COX-2 amplification levels; 50 µM and 90 µM ATRA doses administered alone caused a decrease in Ki-67 amplification levels; 180 µM and 250 µM ATRA doses administered alone caused a decrease in the amplification levels of the VEGF genes. The 50, 100 and 150 µM doses of carboplatin and the 1.25, 2.5 and 5 nM doses of paclitaxel caused a decrease in the COX-2 level. When looking at the data in general, it was observed that combined applications do not have a reduction effect on gene activations as much as single applications. The triple combination of ATRA 150 µM+paclitaxel 2.5 nm+carboplatin 100 µM caused a reduction on COX-2. The combination of ATRA 50 µM+paclitaxel 2.5 nM+carboplatin 100 µM caused a decrease on IRS, COX-2 and VEGF. carboplatin 100 µM+paclitaxel 2.5 nM combination caused a decrease on COX-2; ATRA 50 µM+carboplatin 100 µM combination caused a decrease on IRS and VEGF; ATRA 150 µM+carboplatin 100 µM combination caused a decrease on COX-2; and ATRA 50 µM+paclitaxel 2.5 nM combination caused a decrease on COX-2 (Figure 7).
Figure 7: 1st chart: Amplification curves of Housekeeping gene (18S rRNA); 2nd chart: Amplification curves of the IRS-1 gene; 3rd chart: Amplification curves of the KI-67 gene; 4th chart: Amplification curves of the COX-2 gene; 5th chart: Amplification curves of VEGF gene
Today, cell culture is accepted as one of the main approaches of therapeutic research. The purpose of pharmacology is to determine the active compounds found in natural elements for drug development. In drug development studies, the pharmacological activities of drug candidates are almost always tested in cell culture first. At this stage, the choice of positive control is important (Ghanemi A, 2015).
Mitochondria are the crossroads in many cellular pathways. Apoptosis is involved in many biological processes and is one of the most frequently used areas of research on cell biology. It is also known as programmed cell death. In order to detect apoptosis, apoptotic cells must be distinguished from other cells. Apoptosis can be accurately detected with the MTT staining method. This method is simple and practical. The standard method for studying and measuring apoptosis is the morphological analysis method. DAPI staining method is frequently used to determine the apoptotic effect morphologically. Caspase chain has an important role in the regulation of apoptosis. The released cytochrome C activates caspase-3 (Kumar N, et al., 2018).
The carboplatin and paclitaxel regimen is considered as the first choice adjuvant therapy in all stages of ovarian cancer and is used in neo-adjuvant therapy in stage 3 and 4 ovarian cancer. Paclitaxel is a commonly used anticancer drug and shows its effect by targeting microtubules. Microtubules function in mitosis and are considered essential for cytoplasmic movement. Paclitaxel acts by preventing cell division and polymerization through microtubules, thus apoptosis occurs. Paclitaxel also has angiogenic inhibitory effects, showing this effect by suppressing VEGF expression. carboplatinum is an anticancer drug from the platinum group. In addition to ovarian cancer, it is also used in testicular and small cell lung cancer. Its mechanism of action is based on its inhibition of replication and transcription. In this way, it triggers apoptosis. Apoptosis acts through the activation of a family of cysteine proteases called caspases. Caspase activation is the key step in the onset of apoptosis. Apoptosis occurs with the activation of caspases such as caspases 3 and 7 (Leslie BR and Franco MM, 2018; Kampan NC, et al., 2015; Fleming GF, et al., 2004; Thigpen JT, et al., 1989).
In our study, carboplatin reduced the viability of Ovcar-3 cells at all doses on the second and third days. When the results of the first day were examined, it was observed that while vitality decreased at low doses, it was observed that vitality increased with higher doses. carboplatin and paclitaxel were used both alone and in combination in our study. In similar studies in the literature, the results are similar to those obtained in our study. The combination of paclitaxel with cisplatin or carboplatin was compared in patients with advanced ovarian cancer in randomized clinical-based studies. It has been observed that the treatment regimen in which carboplatin is used in combination is more tolerable, but there is no difference between the combination therapies in terms of efficacy. According to the results of another study, the viability of cells treated with Docetaxel+carboplatin, docetaxel+PNP-GDEPT and carboplatin+PNP-GDEPT and the combination of three agents was examined. Treatment of Ovcar-3 cells with docetaxel, carboplatin or PNP-GDEPT alone reduced cell viability by 42%, 36% and 22%, respectively, compared to controls. The greater reduction occurred in the case of the combination of all three. Apoptosis was examined in Ovcar-3 cells treated with docetaxel (1.5 nM), carboplatin (20 μM), and PNP-GDEPT alone or in combination, the number of apoptotic cells increased in a time-dependent manner in cells treated with the triple combination. As a result of the analyzes using the early apoptosis marker, the highest efficacy was observed in the combination of three agents. The combination of carboplatin+PNP-GDEPT showed the highest effect following the triple combination. Increased sensitivity of resistant Ovcar-3 cells to docetaxel and carboplatin has been observed when included in PNP-GDEPT combination regimens. It has been established that this occurs through increased apoptosis as a result of down-regulation of genes responsible for the drug resistance mechanism. These data are compatible with those obtained in our study (Singh PP, et al., 2011; Bicaku E, et al., 2012).
In our study, paclitaxel reduced the viability of Ovcar-3 cells on the first and second days at all doses. It was observed that the decrease was more pronounced at doses of 5 nM and above on the second and third days. The results obtained in similar studies are similar to the results of our research. In a study, Multicellular Tumor Spheroids (MCTS) were used as conventional cell culture methods may not fully reflect the clinical features of the disease. paclitaxel showed a much weaker effect in MCTS compared to 2D cultures. Following this process, Licofelone, which is predicted to have a synergistic effect with paclitaxel, was combined with paclitaxel and applied to the cells. The combination has been found to have a significant synergistic effect (Hirst J, et al., 2018).
In our study, it was observed that the combination of paclitaxel+carboplatin showed the most significant effect in the first 24 hours at low doses (2.5 nM and 50 µM, respectively). In the combination of paclitaxel+ATRA, there was no significant decrease in the viability of cells in 24 hours compared to the control group. The reduction was mainly observed on the second and third days, and it was determined that cell viability was significantly reduced when the carboplatin dose was increased while the ATRA dose remained the same.
In another study, paclitaxel was combined with silibinin and applied to ovarian cancer cells. MTT analysis was performed 48 hours after administration to determine the effects of the combination. The results showed that cell proliferation was sharply inhibited by paclitaxel. Combined therapy, on the other hand, had a greater effect than drugs alone. The doses used in combined therapy are lower than the IC50 dose determined for paclitaxel and the IC50 for silibinin. This means that the drugs are used in combination at low doses. However, a greater effect has been observed compared to the use of drugs alone. Cell proliferation dropped to 50% after 48 hours. In addition to MTT analysis, the effect of silibinin and paclitaxel combination on apoptosis was investigated. The P53 and P21 gene expression at different concentrations of the combination of silibinin and paclitaxel showed a significant difference compared to control cells (Asl FP, et al., 2018).
Although the results of our study are similar to those of this study, it has been observed that combined applications are generally not as effective on gene expressions as single applications.
In our study, it was concluded that ATRA is a potential agent that can be used in the treatment of ovarian cancer due to its anticancer effect. It has been observed that it can reduce cell viability more than routinely used cancer drugs, especially at high doses. Studies have shown that ATRA, a vitamin A derivative, strengthens cancer chemotherapy in various ways. ATRA has been shown to increase the effects of different anti-cancer agents with its synergistic effect. The mechanisms of their synergistic effects depend on the tumor and cell type. Examples of these mechanisms are the reduction of PCK, c-myc, E2F and Bcl2 expression. The results suggest that combinations of ATRA and anti-tumor agents are candidates for the development and improvement of anti-carcinogenic therapies (Schultze E, et al., 2018).
In a similar study on the subject, the effects of ATRA on multiple human endometrial cancer cell lines were examined. The results showed that retinoic acid derivative ATRA can have more than one antitumor effect and can be used in the treatment of ovarian cancer (Tsuji K, et al., 2017).
In another study, the relationship between Oct4 expression caused by chemotherapeutics in bladder cancer cells and the development of drug resistance and tumor recurrence was investigated. In particular, it has been determined that treatment with cisplatin increases bladder cancer cells by expressing Oct4. When ATRA was used in the same cells, it was observed that Oct4 was inhibited and sensitivity to cisplatin increased synergistically in bladder cancer cells. In addition, it has been noted that the combination of cisplatin and ATRA is effective in suppressing tumor growth compared to cisplatin alone. In another study, the effect of ATRA on aldehyde dehydrogenase expression and drug resistance on paclitaxel resistant ovarian cancer cell lines was examined. MTT analysis was used to examine the effect of ATRA on drug resistance. Analysis results showed that ATRA decreases aldehyde dehydrogenase expression and decreases chemotherapeutic resistance. These results are consistent with those obtained in our study (Lu CS, et al., 2017; Januchowski R, et al., 2016).
In our study, it was determined that alone or in combination application of ATRA, paclitaxel and carboplatin increase caspase-3 activity. It was observed that the aforementioned increase was more pronounced at the end of 12 hours than at the end of 24 hours. The most significant increase was observed in paclitaxel after 12 hours and in ATRA at the end of 24 hours. This increase in paclitaxel and ATRA is more pronounced than in combined applications.
In a study in the literature, the results of MTT and caspase-3 analysis were examined by combining carboplatin and paclitaxel with another drug. For this purpose, the cells were treated with carboplatin and paclitaxel for 48 hours, followed by the addition of the other drug and a further 24 hours. Cell viability was analyzed by the MTT assay. Treatment of the cells with paclitaxel or carboplatin followed by the addition of the other drug resulted in a significant decrease in tumor cell viability. The results demonstrated the superiority of combination therapy over individual treatments at each dose in cell viability. The interesting finding found here was that the greatest reduction in cell viability occurred at lower doses compared to higher doses. In the same study, expression of annexin V and caspase 3 activity were investigated as apoptosis markers. Significant increases in annexin V expression and caspase-3 activity were detected after carboplatin and paclitaxel treatment. When the agent which is the third member of the combined therapy was added to the combination, a decrease in the increase in caspase-3 activity was observed. Similar determinations were made in our research. An example of this is that ATRA alone is found to be more effective than combinations in caspase analysis. In the analysis of gene expressions in our study, it was observed that the effect recorded in single applications was higher than in combined applications (Wahba J, et al., 2018).
These conditions seem to be the opposite of those obtained in studies on the subject. For this reason, it is considered that there is a need for research directed towards this field.
It is known that angiogenesis induced by VEGF plays a key role in cancer development, especially growth and metastasis processes. The family of Insulin Receptor Substrates (IRS) are proteins involved in the insulin-like growth factor I receptor. IRS-1 supports tumor growth, but the mechanism is not fully understood. Based on data from a large cohort of clinical cancer registries, it has been shown that Ki-67 expression is associated with common histopathological parameters and is an additional independent prognostic parameter for overall and disease-free survival in some cancers. COX-2, catalyzes the first step in the formation of prostaglandins. Nowadays, its role in carcinogenesis has become evident. It affects apoptosis and angiogenesis, and there is a high level of COX-2 expression in cancer cells (Li X, et al., 2018; Inwald EC, et al., 2013; Ghosh N, et al., 2010; Reiss K, et al., 2012).
Conclusion
In our study, ATRA and other agents alone and in combination showed significant anticancer effects in MTT, DAPI Staining and Caspase-3 analyses in Ovcar-3 cancer cell lines. In Real-Time PCR analysis, ATRA and other agents showed similar anticancer effects when applied alone. However, the same effect was not observed when agents combined and this is different from some results in the literature. Researching this subject with new studies will contribute to the literature.
The biggest challenge we face in cancer treatment today is the lack of anticancer drugs with high efficacy, broad-spectrum and low side effects. It is accepted that this problem can be solved with combination therapies. It is considered that the findings obtained in our study support this point.
Data Availability
This article is based on the data obtained from the scientific research project at Osmangazi University (Eskişehir/Turkey). The data obtained from the project is in large volume. Therefore, the data has been shared in different articles. Other articles are also under publication.
References
- Jauregui DL, Eritja N, Davis ML, Guiu XM, Navàs DL. Autophagy in the physiological endometrium and cancer. Autophagy. 2020; 17(5): 1-19.
- Visconti RM, Morea D. Big data for the sustainability of health care project financing. Sustain. 2019; 11(13): 1-17.
- McMullen M, Karakasis K, Rottapel R, Oza AM. Advances in ovarian cancer, from biology to treatment. Nat Cancer. 2021; 2(1): 6-8.
- Kumar BS, Maria S, Shejila CH, Udaykumar P. Drug utilization review and cost analysis of anticancer drugs used in a tertiary care teaching hospital. Indian J Pharm Sci. 2018; 80(4): 686-693.
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018; 68(6): 394-424.
- Jaroch K, Jaroch A, Bojko B. Cell cultures in drug discovery and development: The need of reliable in vitro and in vivo extrapolation for pharmacodynamics and pharmacokinetics assessment. J Pharm Biomed Anal. 2018; 147: 297-312.
- Segeritz CP, Vallier L. Cell Culture: Growing cells as model systems in vitro. Basic Science Methods for Clinical Researchers. 2017; 151-72.
- Mokhtari RB, Homayouni TS, Baluch N, Morgatskaya E, Kumar S, Das B, et al. Combination therapy in combating cancer. Oncotarget. 2017; 8(23): 38022.
- Costantini L, Molinari R, Farinon B, Merendino N. Retinoic acids in the treatment of most lethal solid cancers. J Clin Med. 2020; 9(2): 360.
- Kuchipudi SV, Tellabati M, Nelli RK, White GA, Perez BB, Sebastian S, et al. 18S rRNA is a reliable normalisation gene for real time PCR based on influenza virus infected cells. Virol J. 2012; 9(1): 1-7.
- Ghanemi A. Cell cultures in drug development: Applications, challenges and limitations. Saudi Pharm J. 2015; 23(4): 453.
- Kumar N, Afjei R, Massoud TF, Paulmurugan R. Comparison of cell-based assays to quantify treatment effects of anticancer drugs identifies a new application for Bodipy-L-cystine to measure apoptosis. Sci Rep. 2018; 8(1): 1-11.
- Leslie BR, Franco MM. Carboplatin/paclitaxel induction in ovarian cancer: The finer points. Oncol. 2018; 32(8): 418-424.
- Kampan NC, Madondo MT, McNally OM, Quinn M, Plebanski M. Paclitaxel and its evolving role in the management of ovarian cancer. Biomed Res Int. 2015; 2015(1): 1-21.
- Fleming GF, Brunetto VL, Cella D, Look KY, Reid GC, Munkarah AR, et al. Phase III trial of doxorubicin plus cisplatin with or without paclitaxel plus filgrastim in advanced endometrial carcinoma: A gynecologic oncology group study. J Clin Oncol. 2004; 22(11): 2159-2166.
- Thigpen JT, Blessing JA, Homesley H, Creasman WT, Sutton G. Phase II trial of clsplatin as first-line chemotherapy in patients with advanced or recurrent endometrial carcinoma: A gynecologic oncology group study. Gynecol Oncol. 1989; 33(1): 68-70.
- Singh PP, Joshi S, Russell PJ, Nair S, Khatri A. Purine nucleoside phosphorylase mediated molecular chemotherapy and conventional chemotherapy: A tangible union against chemoresistant cancer. BMC Cancer. 2011; 11(1): 1-15.
- Bicaku E, Xiong Y, Marchion DC, Chon HS, Stickles XB, Chen N, et al. In vitro analysis of ovarian cancer response to cisplatin, carboplatin, and paclitaxel identifies common pathways that are also associated with overall patient survival. Br J Cancer. 2012; 106(12): 1967-1975.
- Hirst J, Pathak HB, Hyter S, Pessetto ZY, Ly T, Graw S, et al. Licofelone enhances the efficacy of paclitaxel in ovarian cancer by reversing drug resistance and tumor stem-like properties. Cancer Res. 2018; 78(15): 4370-4385.
- Asl FP, Asl RP, Khodadadi K, Akbarzadeh A, Ebrahimie E, Pashaiasl M. Enhancement of anticancer activity by silibinin and paclitaxel combination on the ovarian cancer. Artif cells nanomedicine Biotechnol. 2018; 46(7): 1483-1487.
- Schultze E, Collares T, Lucas CG, Seixas FK. Synergistic and additive effects of ATRA in combination with different anti-tumor compounds. Chem Biol Interact. 2018; 285: 69-75.
- Tsuji K, Utsunomiya H, Miki Y, Hanihara M, Fue M, Takagi K, et al. Retinoic acid receptor β: A potential therapeutic target in retinoic acid treatment of endometrial cancer. Int J Gynecol Cancer. 2017; 27(4): 643-650.
- Lu CS, Shieh GS, Wang CT, Su BH, Su YC, Chen YC, et al. Chemotherapeutics-induced Oct4 expression contributes to drug resistance and tumor recurrence in bladder cancer. Oncotarget. 2017; 8(19): 30844.
- Januchowski R, Wojtowicz K, Sterzyſska K, Sosiſska P, Andrzejewska M, Zawierucha P, et al. Inhibition of ALDH1A1 activity decreases expression of drug transporters and reduces chemotherapy resistance in ovarian cancer cell lines. Int J Biochem Cell Biol. 2016; 78: 248-259.
- Wahba J, Natoli M, Whilding LM, Parente-Pereira AC, Jung Y, Zona S, et al. Chemotherapy-induced apoptosis, autophagy and cell cycle arrest are key drivers of synergy in chemo-immunotherapy of epithelial ovarian cancer. Cancer Immunol Immunother. 2018; 67(11): 1753-1765.
- Li X, Gao Y, Li J, Zhang K, Han J, Li W, et al. FOXP3 inhibits angiogenesis by downregulating VEGF in breast cancer. Cell Death Dis. 2018; 9(7): 1-12.
- Inwald EC, Schalke MK, Hofstädter F, Zeman F, Koller M, Gerstenhauer M, et al. Ki-67 is a prognostic parameter in breast cancer patients: Results of a large population-based cohort of a cancer registry. Breast Cancer Res Treat. 2013; 139(2): 539-552.
- Ghosh N, Chaki R, Mandal V, Mandal SC. COX-2 as a target for cancer chemotherapy. Pharmacol Reports. 2010; 62(2): 233-244.
- Reiss K, Del Valle L, Lassak A, Trojanek J. Nuclear IRS‐1 and cancer. J Cell Physiol. 2012; 227(8): 2992-3000.
Author Info
Hulusi Goktug Gurer1, Ceren Yildiz Eren1*, Ozlem Ozgür Gursoy1, Ayşe Tansu Koparal2 and Sabit Sinan Ozalp32Department of Medical Services and Techniques, Anadolu University, Eskisehir, Turkey
3Department of Obstetrics and Gynecology, Eskişehir Osmangazi University, Eskisehir, Turkey
Received: 07-Jul-2021 Accepted: 21-Jul-2021 Published: 28-Jul-2021
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3