Review Article - (2022) Volume 13, Issue 2
Abstract
This case is of a young female with a large uterine leiomyoma causing phlegmasia cerulea dolens with thrombosis of the left common and left external iliac veins. She underwent mechanical thrombectomy to temporize the condition until she could be evaluated by gynecology- oncologist to remove the cause of venous obstruction.
Keywords
Phlegmasia, Uterine leiomyoma, Thrombosis
Introduction
Uterine leiomyomas are the most common pelvic tumor, found in pre-menopausal women (Stewart EA and Tommaso SKL, 2019). There have been reports of leiomyomas causing compression of the right common iliac vein and subsequent development of Deep Vein Thrombosis (DVT). We report a young female who presented with phlegmasia cerulea dolens secondary to compression of the left common iliac vein by a large uterine leiomyoma. She underwent mechanical thrombectomy to temporize her condition prior to total abdominal hysterectomy. Informed consent was obtained for all procedures and publication of this case report, including all accompanying images (Plate G, et al., 1984).
Case Description
A 46 year old female presented to the emergency department with complaint of left lower extremity pain of two days duration. Swelling originated around the ankle with progression to the groin. Medical history was significant for oral contraceptive use and a known uterine leiomyoma, approximately 10 cm at last evaluation. Physical exam revealed left lower extremity swelling extending from foot to mid-thigh with erythematous discoloration of skin (Figure 1). Biphasic Doppler signals in left posterior tibial and dorsalis pedis arteries were present with triphasic signals on the right side. Motor and sensory function was intact in both lower extremities.
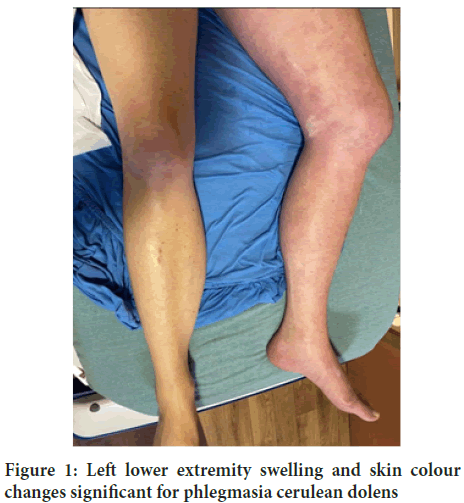
Figure 1: Left lower extremity swelling and skin colour changes significant for phlegmasia cerulean dolens
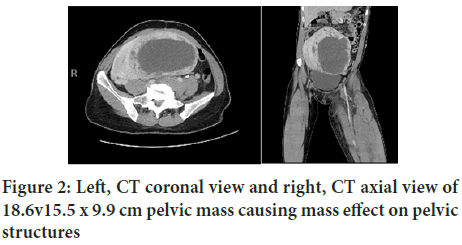
Duplex venous imaging showed extensive acute DVT of the left common femoral, femoral, popliteal, gastrocnemius, posterior tibial, peroneal, and great saphenous veins. The left External Iliac Vein (EIV) close to the junction with the Common Femoral Vein (CFV) showed evidence of thrombosis. However, the left Common Iliac Vein (CIV) could not be evaluated with duplex venous imaging. Computed Tomography (CT) pulmonary embolism protocol showed right lower lobe segmental and subsegmental emboli. CT venogram of abdomen and pelvis showed a large heterogenous mass which measured 18.6 × 15.5 × 9.9 cm (Figure 2). Mass effect was noted on the Inferior Vena Cava (IVC) and left CIV with evidence of thrombus in the left EIV, Internal iliac vein, and CIV. Ankle-brachial indices were not obtained. She was started on intravenous heparin.
Figure 2: Left, CT coronal view and right, CT axial view of 18.6v15.5 x 9.9 cm pelvic mass causing mass effect on pelvic structures
A left lower extremity venogram with access through the left popliteal vein, demonstrated thrombus within left femoral and common femoral veins and chronic near complete occlusion of the left EIV and the entire portion of the left CIV. A 30 cm infusion length UniFuse catheter (Queensbury, N.Y.) was placed with the treatment area from proximal IVC to the distal femoral vein. Overnight, thrombolysis was initiated with Tissue Plasminogen Activator (tPa).
The Infusion catheter was removed after 12 hours. Left lower extremity venogram demonstrated persistent thrombus within the left femoral vein. There was persistent lack of flow within the distal left external iliac vein and the left CIV.
Angioplasty, with a 4 × 40 mm Armada balloon (Abbott Park, IL.) was performed within the IVC, left CIV and EIV for purposes of pre-dilatation prior to mechanical thrombectomy with the Inari, a 105 cm × 16 mm Clottriever (Irvine, CA.), in order to gain access into the lumen. Mechanical thrombectomy of the proximal IVC left CIV, EIV, common femoral and femoral veins with retrieval of a large amount of acute, subacute and chronic appearing clot (Figure 3).
Figure 3: Top left, imaging after tPa, prior to mechanical thrombectomy; Top right, imaging after mechanical thrombectomy; Bottom, thrombus extracted using Inari device
A completion venogram demonstrated complete removal of the thrombus within the left femoral, common femoral and the visualized portions of the proximal EIV. Flow was present within the left CIV with contrast seen entering the IVC. There was chronic stenosis of the left CIV and EIV secondary to mass effect of the uterus.
A suprarenal Option-Elite IVC filter (Athens, TX.) was placed prior to surgery for excision of pelvic mass. Systemic heparin was held 6 hours prior to surgery. She underwent total abdominal hysterectomy with bilateral salpingectomy, with preservation of normal ovaries. Pathology showed the mass to be a large benign leiomyoma measuring 18 × 18 cm.
Approximately eight hours postoperatively the patient started complaining of recurrent left calf tightness and swelling. Increased pitting edema with palpable pulses, compartments was soft and no pain with passive range of motion. Repeat US duplex showed acute DVT of left common femoral, femoral, posterior tibial, and peroneal veins.
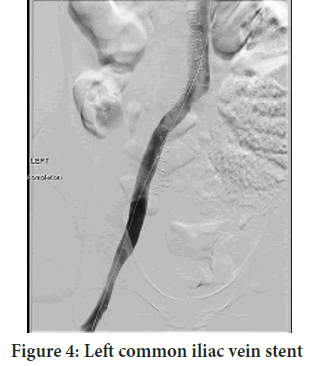
Venogram showed diffuse thrombosis of the left femoral, common femoral, external and common iliac veins with high-grade stenosis involving the common iliac vein. Mechanical thrombectomy was repeated with the Inari Clottriever (Arko FR, et al., 2007; Beyth RJ, et al., 1995). The venogram did not show residual thrombus. Intravascular ultrasound demonstrated an 80% stenosis involving the mid to distal left CIV that was likely missed on prior imaging due to overlying thrombus. Balloon angioplasty with a 14 mm Atlas balloon was performed within the common iliac vein, followed by placement of a 16 × 120 mm Boston Scientific Vici stent (FDA, 2021) Completion venogram demonstrated adequate inflow and outflow through the left common iliac vein stent with no significant residual thrombus or stenosis (Figure 4).
Figure 4: Left common iliac vein stent
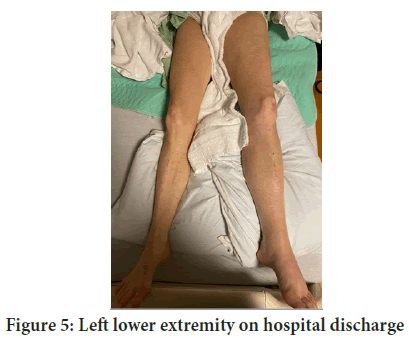
Her post-operative course was complicated by adynamic ileus that resolved with conservative management. She required blood transfusion due to steady drop in her hematocrit. CT arteriogram of abdomen and pelvis showed large pelvic hematoma with extravasation. However, angiography failed to show active bleed, likely caused by missed bleed during hysterectomy. Anticoagulation was held until hemoglobin stabilized. She was discharged on hospital day 15 on oral Apixaban 5 mg twice daily. Her left lower extremity edema had much improved, (Figure 5). She returned two months later and had the IVC filter retrieved. Follow up office visit three months later showed patient left CIV and EIV stent.
Figure 5: Left lower extremity on hospital discharge
Results and Discussion
Phlegmasia Cerulea Dolens (PCD) is a precursor of venous gangrene. It is a limb and life threatening condition with a mortality of 20-40%, and 30% of those deaths caused by pulmonary embolism (Chaar CIO, Satoskar S, 2019). DVT is diagnosed in about two million Americans every year, but PCD is rare. PCD is also known as “milk leg” due to its association with third trimester pregnancy and postpartum state, even though it is more prevalent in men with a ratio of 1.5:1 (Weaver FA, et al., 1988). Patients present with pain followed by significant swelling and cyanosis secondary to collateral vein involvement, causing massive fluid shift into interstitium, obstruction of arterial flow, and ultimately capillary involvement leads to venous gangrene (Reddy MHK, et al., 2016).
May-Thurner Syndrome (MTS), is compression of the proximal segment of the left CIV by the right common iliac artery, it is rarely the differential for acute DVT, although can be associated with chronic thrombus. The most common variant found in about 20% of the population is the compression of the left iliac vein by the right iliac artery against the lumbar spine causing collagen deposition in the vein known as venous spurs (May R and Thurner J, 1957). Consequential venous stasis increases the risk of DVT.
Risk factors for MTS overlap with the risk factors for DVT. These include female gender, especially those using oral contraceptives or in the postpartum period, scoliosis, and thrombophilias. This case did not involve this anatomic defect of compression of iliac vein by iliac artery, but instead was caused by the direct compression of left iliac vein by enlarged fibroid uterus.
Conclusion
Patients with DVTs are generally placed on systemic anticoagulation to prevent further thrombosis. In this case, catheter directed thrombolysis as well as mechanical thrombectomy was utilized until hysterectomy with bilateral salpingectomy was performed, addressing the etiology of this extensive DVT. There have been several case reports of uterine mass causing occlusion to venous flow. However, it is difficult to effectively treat the phlegmasia and venous thrombosis without treating the underlying cause, such as pelvic mass.
References
- Stewart EA, Tommaso SKL. Uterine leiomyomas (fibroids): Epidemiology, clinical features, diagnosis, and natural history. UpToDate. 2019.
- Plate G, Einarsson E, Ohlin P, Jensen R, Qvarfordt P, Eklof B. Thrombectomy with temporary arteriovenous fistula: The treatment of choice in acute iliofemoral venous thrombosis. J Vasc Surg. 1984; 1867-876.
[Crossref] [Google scholar] [Pubmed]
- Arko FR, Davis CM, Murphy
EH, Smith ST, Timaran CH, Modrall JG. Aggressive percutaneous mechanical thrombectomy of deep venous thrombosis. 2007; 142(6): 513-519.[Crossref] [Google scholar] [Pubmed]
- Beyth RJ, Cohen AM, Landefeld CS. Long-term outcomes of deep-vein thrombosis. Arch Intern Med. 1995; 1551031-1037.
[Crossref] [Google scholar] [Pubmed]
- Boston scientific corporation recalls vici venous stent system and vici rds venous stent system for potential of stent migration. FDA. 2021.
- Chaar CIO, Satoskar S. Phlegmasia alba and cerulea dolens. Background, pathophysiology, epidemiology. Medscape. 2019.
- Weaver FA, Meacham PW, Adkins RB, Dean RH. Phlegmasia cerulea dolens: Therapeutic considerations. South Med J. 1988; 81(3): 306-312.
[Crossref] [Google scholar] [Pubmed]
- Reddy MHK, Sangeetha B, Aruna M, Chandra VS, Kumar ACV, Ram R, et al. Phlegmasia cerulean dolens:
Complication of femoral vein catheterization. CEN Case Rep. 2016; 5(2): 184-187.[Crossref] [Google scholar] [Pubmed]
- May R, Thurner J. The cause of the predominantly sinistral occurrence of thrombosis of the pelvic veins. Angiology. 1957; 8(5): 419-427.
[Crossref] [Google scholar] [Pubmed]
Author Info
Elisabeth Ekkel*, Tara Chandran, Ryan Qasawa, Michael Trpkovski, Sachinder Hans and Henry Ford MacombCitation: Ekkel E: Management of Phlegmasia Cerulea Dolens Caused by a Giant Leiomyoma
Received: 07-Feb-2022 Accepted: 21-Feb-2022 Published: 28-Feb-2022, DOI: 10.31858/0975-8453.13.2.87-89
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3