Research Article - (2022) Volume 13, Issue 3
Abstract
Today, sociodemographic factors and lifestyle habits more affect body weight and body composition. Obesity is the imbalance of energy intake from food and energy expended through physical activity. Globally it affects ≥ 135 million people in India and in US 39.8% of adults and 18.5% of youth. Obesity exaggerates many major problems which is untreatable. Screening of obesity can be done by body mass index and other methods. Variates of medication are used in management of obesity. It has been already proved in various clinical trials that there are various drugs are used for treatment of obesity with some modification in life style, diet and behavioral modification. Orlistat has been found most desirable drug to manage obesity. In sever condition some time various surgical operation can be performed over patient to reduce morbidity. In this review we can see how to manage obesity by pharmacological and non-pharmacologically because obesity is a global concern as it arises many health disasters and expected to accentuating in future, among rural and older individuals. Although in recent last years it has been clearly showed that being overweight puts high risk of dying from COVID-19 as it increases oxygen demand, ventilators etc. so it is a like a wakeup call to come in action by introducing new campaign. So, government, health workers, researcher have to take urgent steps regarding management and treatment in obesity.
Keywords
Obesity, Behavioral modification, Body mass index, Management, Diet
Introduction
Obesity has become a worldwide problem related to major chronic public health issues and increases threat to the health of many people that affect the quality of life increases the risk of illness and health care cost. Obesity, a condition common nutritional disorder which is characterized by excess body fat (Pozza C and Isidori AM, 2018). It is gradually increases globally. It aggravates many health conditions such as, hypertension, dyslipidemia, type 2 diabetes, cardiovascular disease and sleep apnea, symptomatic heart burn, fatty liver, gall stones, abdominal wall hernias, post-operative problem, osteoarthritis, depression and psychotic problem etc. (Kyrou I, et al., 2018). It has been reported that in US 2/3rd of the people (adults) and in 2003 to 2004 about 4.8% people were obsessed. India has acquired 3 places after US and china about 30% people were obsessed and 15% obsessed people live in India together with China. Standard data has been reported for obesity with comparison of south India 46% (women-47% and 43%-men) to USA 35%. Abdominal obesity has been found 47% to 51% in women with higher rates (women-56% and men 35%) and greater risk for developing type-II diabetes and heart related disorders (Ogden CL, et al., 2015). Today obesity is only reason for heightens one or more than one health conditions such as type-2 diabetes, heart related disorders certain cancers which increases the severity of the obesity crisis. Development of insulin resistance type-2 diabetes mellitus are the major problems which occurs during obesity so it is considered that it is a major obstacle to maintain long term body glucose level (Calle EE, et al., 2003; van Gaal LF, et al., 2006). It has been seen that more than 90% people suffers from type-2 diabetes having obesity in various clinical trial study has been demonstrated that increase in 6-7 kg body weight has been increases the risk of type-2 diabetes by 50% while loss in 5 kg reduces the risk as similar. As a result, people having Body Mass Index (BMI) ≥ 40 kg/m2 suffer from type-II diabetes (Mokdad AH, et al., 2003). Several surgeries, non-pharmacological, pharmacological method has been used to control obesity. There is a strong evidence exist that bariatric surgery leads to greater loss in weight and has been seen positive effect on fasting blood sugar, hemoglobin A1c, lipid profiles (Gadde KM and Allison DB, 2009).
Researchers have found that there are several risk conditions which are associated with obesity are diabetes mellitus, coronary artery disease, hypertension, dyslipidemia, stroke, osteoarthritis, gall balder and several cancers etc. Therefore, it has been proved that obesity increase risk of morbidity (Jakobsen GS, et al., 2018).
In 1997 World Health Organization (WHO) was published the classification of adults on the basis of Body Mass Index (BMI). This classification has been proposed cut-of points for BMI. For low BMI it is <18.5 kg/m2 and for high BMI it is >40.0 (for obesity stage III) (WHO, 2015; WHO, 1997) (Table 1).
| Classification | BMI | Stage of obesity | People health description |
|---|---|---|---|
| Underweight | ˂18.5 kg/m2 | - | Thin |
| Normal | 18.5-24 kg/m2 | - | Healthy/normal |
| Overweight | 25-29.9 kg/m2 | - | Overweight |
| Obesity | 30-34.9 kg/m2 | Ⅰ | Obesity |
| 35-39.9 kg/m2 | Ⅱ | Obesity | |
| Extremely obesity | ≥ 40.0 kg/m2 | Ⅲ | Morbid obesity |
Table 1: Classification of obesity by Body Mass Index (BMI) adapted from obesity, preventing and managing the global epidemic WHO 1997
Valuable information was provided by BMI Obesity classification, it talks about increasing body fatness and compared weight status between population and within population and also provides data of groups of individuals at risk of morbidity and mortality (Han TS, et al., 2006).
Assessment of obesity
Obesity screening should be initiate with a determination of the BMI. It is just an indicator for health risk. A World Health Organization (WHO) classified overweight and obesity for both men and women. In 1997, classification made by WHO (Table 2). BMI have been defined as weight in kilogram divided by square of the height in meters (WHO, 2015; WHO, 1997). According to National, Heart, Lung and Blood Institute (NHLBI) physician also looks for another factor. Second assessment of obesity is waist circumference (NIH, 1998; ICSI, 2011) defined as measured in centimeter at midpoint between lower border of ribs and upper border of the pelvis and it also provide measurement for assessing upper fat deposition, neither provide precise estimates intra-abdominal visceral fat. Abdominal adiposity is important risk factor for Type 2 diabetes, cardiovascular disease, dyslipidemia, hypertension (Bray GA, 2013). It has been seen that having greater waist circumference have increase five-fold more chances of multiple disease, such as cardiovascular risk factor and others. It has been shown that patient having BMI 25 kg/m2 or greater and waist circumference >35(women) and >40(men) have greater risk of blood pressure, lipid level, fasting glucose, coronary heart disease, atherosclerotic disease, type 2 diabetes (Ghandehari H, et al., 2009; CDC, 2013; Westphal AB, et al., 2010). Any of three or more risks factors confirms high morbid obesity. Another assessment skin fold thickness, defined as measurement of skin fold thickness in centimeter with calipers which provide a precise assessment if taken at multiple sites and it don’t provide any information about abdominal and intra muscular fat (Kannieappan LM, et al., 2013). Another assessment is bio impedance, defined as the lean mass conduct current better than fat mass because it was primarily an electrolyte solution. It also measured a resistance to a weak current (impedance). Applied across extremities and provide an estimation of a body fat by help of using empirically derived equation. Benefit of bio impedance is that the method used in measurement is very simple and practical but it never measured fats and nor predict biological outcomes (Tarnoki AD, et al., 2014).
| Classification | Obesity stage | Disease risk on the basis of waist circumference | |
|---|---|---|---|
| Men˂40 women < 35 | Men>40 women >35 | ||
| Underweight | - | - | - |
| Normal | - | - | - |
| Overweight | - | Increases | High |
| Obesity | Ⅰ | High | Very high |
| Ⅱ | Very high | Very high | |
| Extremely obesity | Ⅲ | Extremely high | Extremely high |
Table 2: Classification of obesity by waist circumference and associated diseases risk adapted from obesity preventing and managing the global epidemic WHO 1997
Materials and Methods
Epidemiology of obesity
Today the scenario is completely different in comparison to last few days. The number of people who are suffering from the obesity and obesity related disorder has nearly double. World health organization (WHO) estimated that from year 1980-2013 obesity rates have been increased by 47.1% and also found in 2014, approximately 41 million children under age of 5 year were affected by overweight and obesity (WHO, 2016). On national level studies of US children and adolescent obesity from age group 2-19 years were 17% in 2011-2014. But extreme obesity was found to be 5.8% (Ogden CL, et al., 2016) according to NCHS (National Center for Health Statistics) data from CDC (Center for Disease Control) prevalence of obesity among US youth and adults was found to be 18.5% and 39.8% in 2015-2016 (Hales CM, et al., 2017). It has been seen that the percentage of obesity in men age group between (40-59) are 40.8 and men age group of (20-30) are 34.8% and on the other hand women age (40-59) are 44.7% and women age group (20-39) are 36.5%. This data proves women are more affected by obesity. From most of the recent studies it was found in United States overall of 18.5% of youth and 20.6% of adolescent has been obese. About 18.4% of school aged children were affected by obesity with compare to pre schooled aged children (13.9%). further 20.4% of school aged boys are getting more effected then pre schooled aged boys (14.3%), same case was found in girls also. About 20.9% of adolescent girls were more affected by obesity then pre schooled aged girls (13.5%) (Hales CM, et al., 2017) from (1999-2000) to (2015-2016) about 13.9% of obesity among youth between aged group (2-19) years has been increased to 18.5% (Hales CM, et al., 2017).
According to National Health and Nutrition Examination survey in (US) on the basis of body mass index classification shows that there was a steady increment in prevalence of obesity in both children and adults. About 35.8% of adults and 18.5% of youth in 2015-2016 were obese (WHO, 2008) from 1980 to 2014 current scenario trends of obesity on worldwide prevalence of overweight and obesity has been become doubled and reached to 1.9 billion people were overweight and 600 million people were obesity (WHO, 2014).
Overall past three four decades obesity was gradually increased worldwide among adults in aged group 18 year about 11% of man and 15% of women were obese in 2014. In 2013 children under age of 5 years about more than 41 million children were overweight (IIPS, 2000).
In India it was observed from (1998-1999) to (2015-2016) the BMI was gradually increased from 20.3 kg/m2 to 21.9 kg/m2 which signify that from last decade obesity and overweight was roses. Mean BMI has increased in age group of (30-39) and (40-49) year of women. In comparison of community Muslim women were more affected by obesity than Hindu women (IIPS, 2009). If we study properly, it has been also showed that scheduled caste women were more affected by obesity and overweight. The mean BMI of schedule caste women in 2015-2016 were found to be 21.8 kg/m2 but in 1998-1999 it was 20.1 kg/m2 which indicate that this was significant changes. In other hand there was also significant change was observed in mean BMI of upper wealth quintiles women in 2015-2016. In total if we compare overall obesity in women, it has been doubled from (1998- 1999) to (2015-2016). In (2015-216) 20% of women were obese whether in 1999 it was only 10.6% which shows gradually increment in obesity in last two decade (Devaux MG, et al., 2017). If we talk about particular age 30-39 year age group women were more affected and it reaches to 27.7% in (2015-2016) from 7.3% in (1998-1999). On comparing married with non-married, married women were more affected by obesity among both rural and urban areas. Educating system also gave more powerful impact on obesity prevalence. It gives positive attributes to obesity. Higher increment in level of obesity was found among in illiterate women and up to primary school education. But now obesity trend was tripled from 1998- 2016 among scheduled tribes, scheduled caste and other backward caste (Frech HE, et al., 2014).
In current scenario, it has been shown that, more than one out of two adults and one out of six children were obese in OECD area/countries. To solve the obesity problem there are some strategies and planning are merged in label of foods to improve nutrient information by means of news media, social sites, etc. (especially by communication). It helps to empower people to makes better choices of food product. In 2000, according to health behavior in school aged children survey in OECD 15th year old children are gradually increases their weight in France and children age of (3-17) year were at stable rate but in England it was increases for boys and girls (Kaur S, et al., 2005).
OECD (organization for economic co-operation and development) is an intergovernmental economic organization with 36 member countries, founded in 1961 to stimulate economic progress and world trade (Palamara KL, et al., 2006). According to OECD, in 2015 about 19.5% adult were obese. This data varies with countries. In Korea and Japan (<6% adult) and in countries like Hungary, New Zealand, Mexico and the United State (>30% adult) were obese. This range increases sharply in England, Mexico and United State since past (1990). In other seven OECD countries this rate has been slower than other countries which were described above. In countries, Canada, Frence, Mexico, Switzerland and the United State, obesity range increases and this rate constant in England, Italy, Korea, Spain. This shows that, there is no reduction in obesity rate (Frech HE, et al., 2014). In India among (11-19) age, obesity has been found vary high (11%-29%). In rural area 4.7% of adolescence suffer from obesity but in urban’s area it was found to be 11.6% so this prove urban area people were more suffer from obesity due to changes in life style, socioeconomic condition etc. according to recent data in Pune and Maharashtra, in the age group 10-15 year, total 1228 boys were overweight (20%) and 5.7% were obese (USDA, 2008). In 2002, survey was done on a school child of Ludhiana, Punjab total prevalence of overweight were 11%-14%, in age group 9-15 years. In other hand similar survey was done by nutrition foundation of India among 5000 private school children and 29% of 4 to 18 years age groups affected and overweight and a similar study was conducted in Chennai and founded 17% were over weighted and 3% were obese (USDA, 2008).
Management of obesity
Management of obesity is done by different method. It is classified as non-pharmacological and pharmacological method.
Non-pharmacology: It includes various strategies and planning to manage obesity.
Diet and Behavior modification: There are integrated Programmed regarding diet which include how much calorie intake, fat restriction, daily workout and life style. The goal of this integrated programmed is to reduce 5%-10% body weight (USDA, 2008). Sometime nutrition counselor may also help to plan a healthy diet which increases patient compliance in first year after drug therapy. Nutrition counselor must need to find out history of nutrition and physical activity of patient to helping out from overweight and to adapt healthier behavior on daily basis. Counselor provides a diet plan and daily calorie intake for an effective weight loss. The academy of nutrition and dietetics is an important resource for finding a registered dietitian (Potter MB, et al., 2001; Bray GA, 2013).
For effective weight loss counselor provide low-carbohydrate and low-fat diet otherwise, best diet is only those patients will able to follow it constantly. According to National Heart, Lung and Blood Institute (NHLBI) guidelines to effective weight loss the amount of calorie intake should be reduce from 500-1000 kcal/day (LeBlanc ES, et al., 2011). According to the dietary guidelines for Americans 2005, the person whose weight more than 154 pounds (70 kg) are burned more calorie/hour in comparison to person weight less than 154 pounds. For effective weight loss it is necessary to loss (1-2) pound/week and also reduce in 500-1000 by taking low calorie in a meal or increase energy expenditure (Potter MB, et al., 2001). Physical activity is the only means of energy expenditure. According to USPSTF, 2010 6% decrement in weight has been observed by the behavioral treatment (Bray GA, 2013; LeBlanc ES, et al., 2011). USPTF developed 5A’s approach to manage obesity and body weight for the patient who are not hesitating and ready to change in their life style (Figure 1). According to National Weight Control Registry, self-monitoring is key element for improving behavioral weight loss programmed. It Includes food diaries, physical activity and weight records. In conjugation with dietary and drug therapy it is more effective for weight loss (Rao G, et al., 2010; Searight HR, 2009).
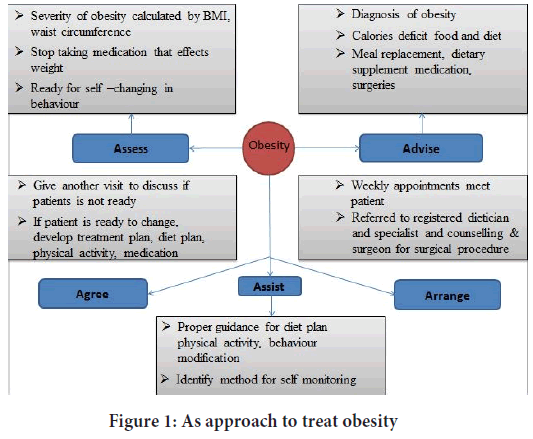
Figure 1: As approach to treat obesity
Motivational interviewing: Motivational interviewing is a focused, goal directed and counselling approach for behavioral change by helping patients to explore and resolve equivocation. It is best method for the people who willingly accept to reduce their body weight. Component of motivational interviewing include, agenda setting exploration about patient desire, patient ability, patient reasons, information, listening and summarizing and generating option and contracting etc. (Pollak KI, et al., 2011; Janssen I and LeBlanc AG, 2010).
Physical activity: Physical activity is defined as energy expenditure by movement of skeletal muscles. It can be performed any time of day or night. It may be planned or unplanned, and repetitive process for the purpose of improving body fitness (Coleman KJ, et al., 2012). Physical activity helps in to balance both physical and mental health and may prevent from risk factors for several diseases which may threat life. It also increases stamina, strength, builds healthy bones, muscles and reduces some mental stress. It may help to increase self-esteem in children and adolescent (ODPHP, 2013). NHLBI has been suggested, 30-45 min daily physical workout is necessary in 3-5 days in a week. Daily workout is also necessary in maintaining metabolic rate, which help to lowering blood pressure and cholesterol level (Potter MB, et al., 2001). The American college of sports medicine has took an initiative for assessment of physical activity to be considered as a vital step to remains fit in to daily routine for maintaining a healthy life. The physical activity guidelines for Americans (2008) set a parameter for adults to perform at least 150 min of moderate intensity or 75 minutes of vigorous intensity aerobics activity per week to remain fit in a daily life (Coleman KJ, et al., 2012; ODPHP, 2013). In moderate physical activity include, hiking, light gardening, dancing, bicycling, walking, weight lifting, and stretching expanded 370 kcal, 330 kcal, 330 kcal, 290 kcal, 280 kcal, 220 kcal, and 180 kcal energy approximately per hour. But in case of vigorous physical activity daily calorie expended in bicycling, walking, aerobic are 590 kcal, 460 kcal, 480 kcal approximately (Potter MB, et al., 2001).
Mental health and mood: The mental health of people is related to healthy behavior in which include eating pattern, and participation in type of physical activity. Mental health and mood behaviors gives powerful impact on weight and obesity it has been seen that people having greater BMI are more affected by depression, anxiety in comparison to a healthy people or children. In several researches it has been proved that reducing level of stress used as a potential factor to minimize obesity (Rofey DL, et al., 2009; Anderson SE, et al., 2007).
Sleep hygiene: About 17 million children in the age group 6-17 years affected with obesity due to inadequate sleep and children up to 4 years of age increase 2 times more chances of obesity and overweight due to lack or short duration of night time. It also found that due to inadequate sleeping less than 7.75 hours/day in girls increases 4 times more risk of obesity and in boys 1.6 fold increases risk of obesity (Bell JF and Zimmerman FJ, 2010; Mcketta S and Rich M, 2011).
Media usage: According to recent study, it is found that children are spend more time on television, computers, videogames which increases more chance of obesity by increases body fatness, decrease energy expenditure, less physical activity etc. (Andrews RA and Lim RB, 2013).
Surgical method: Bariatric surgery is one of the methods to manage sever condition of obesity particularly when there are several risk factors are associated and it may threat to life. Patients having more than 40 kg/m2 body weight are more preferred for bariatric surgery (SAGES Guidelines Committee, 2009). Bariatric surgery has become an option when dietary, nutrients, physical workout, and medication have not produced suitable results. Bariatric surgery has been opted when patients with BMI 35 kg/ m2 or more with chances of sever disease such as diabetes, sleep apnea, joint diseases etc. (Sjöström L, et al., 2007). The Swedish Obese Subjects study suggested, replacement of open surgery by laparoscopy resulting in 24% reduction in mortality because of reducing the chance of myocardial infarction and cancers. Weight loss surgery can be opted by two method gastric restrictions and malabsorption or both. It involved small change in digestive system by limiting amount of food (Shah K, et al., 2016; Pucci A, et al., 2018).
Rouxen-en-y: It is also known as gastric bypass, most common, non-reversible method in U.S. This type of surgery involved by limiting the amount of food and lowering absorption of nutrients. In this surgery makes a small cut on the top of stomach and sealed it and small portion of small intestine is bypassed resulting only ounce of food can be holed by stomach. And it also increases energy expenditure (Levine MS and Carucci LR, 2014). It leads to 60% to 70% weight are loss by patients in 9 to 14 months after surgery. But there are several disadvantages have been seen in this surgery. It requires more complex operation, and need to stay more time in hospital. After surgery it is required to take long time vitamin, mineral supplement because of deficiencies of vitamin B12 iron, calcium etc. (Novikov AA, et al., 2018; Goitein D, et al., 2016).
Sleeve gastrectomy: In sleeve gastrectomy surgery about 80% of stomach has been removed only leaving a suitable pouch so that it can’t hold much food resulting less amount of production of appetite regulating hormone ghrelin. This type of surgery is non-reversible and gives rapid and significant weight loss and no need to stay longer time in hospital. But after surgery long term of vitamin deficiencies has been seen (Lara MD, et al., 2005; Puzziferri N, et al., 2014).
Adjustable band: It is most invasive method. This procedure is almost same as sleeve gastrectomy. Only difference is another one surgery has been done to connect the end portion of intestine to duodenum which limits amount of food and reduces absorption of nutrients and produces another risks factor like malnutrition and vitamin deficiencies. It is also known as biliopancreatic diversion with duodenal switch. This method of surgery gives greater weight loss in comparison to others method. Patients are allowed to eat normal diet and meals. This method is not effective in case of diabetic patients. Sometime this produces high complication rate and need to stay longer time in hospital (Snow V, et al., 2005).
Laparoscopy surgery: Laparoscopy surgery is only applicable for sever condition of obesity. It involved special type of telescope which is known as laparoscope, to view the stomach. It is a simple operative procedure having low risk. This surgery required a small cut in stomach along its vertical axis, a plug of stomach has been removed from a distal part for creating a durable reinforced and rate-limiting stoma and from this hole propylene is placed and stapled to it-self. This method avoids large open incision leads to fewer blood loss and pain (Leung WYS, et al., 2003). This method required anesthesia during surgery and sometime may produces sore throat and nausea. After surgery it is necessary to monitor daily habits of patients. Patients should need to rest and take proper supplements. Daily walking and first liquid diet followed by solid food is more preferable for patients to fast recovery (Li MF and Cheung BMY, 2011).
Results and Discussion
Obesity treatment by drugs
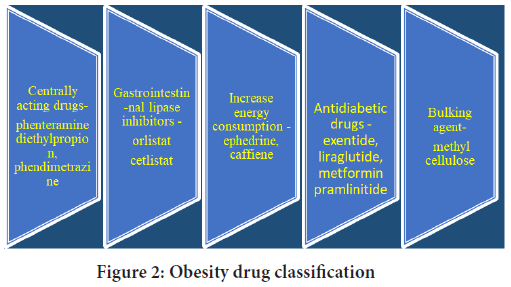
The treatment of obesity by means of medication has withdrawn kind attention from doctors and patients because of shown in improvement of insulin sensitivity, glucose level, lipid level and hypertension in obese patients (Kaplan LM, 2010). The main aim of obesity treatment and management has been to lowered the cardiovascular risk factors so that the overweight and obesity related morbidity and mortality can be reduced. So that use of different medication has given more benefits with reduced mortality and morbidity (Li MF and Cheung BMY, 2011). Anti-obesity drugs can be classified in to following categories: Drugs that reduce fat absorption; centrally acting drugs (anorectic drugs); drugs that increases energy expenditure; antidiabetic drugs and bulking agents (Hendricks EJ, 2017; Rebello CJ, et al., 2018) (Figure 2).
Figure 2: Obesity drug classification
Anorectic drugs reduce food intake by acting on central nervous system. It includes noradrenergic, adrenergic and serotonergic drugs bind with the GABA receptors or cannabinoids receptors. Noradrenergic drugs block the uptake of noradrenalin from presynaptic vesicles into neurons to decrease food intake by acting on beta adrenergic receptors. It includes diethylpropion, phentermine, amphetamine etc. but these drugs have been withdrawn from market due to increased hemorrhagic stroke and amphetamine produces addiction so that it is not in use (Bray GA, 1993). In combination of lifestyle modification phentermine gives insignificant results in weight loss about 3.6 kg in 6 months. In comparison of diethylpropion, phentermine gives better results. The combine effect of phentermine andtopiramate was started in September 2012 gives synergistic effect with reduction in dose and produced less toxicity without loss in efficacy (Henness S and Perry CM, 2006; Demos LL, et al., 2006).
Drugs reduces intestinal fat absorption
Orlistat has been only weight-loss drug that only approved by the FDA. It is reversible gastrointestinal lipase inhibitor which inactivates hydroxylation of dietary fat and prevents absorption of dietary fats, which results in thirty percent reduction in fat absorption has been absorbed in the gut (Müller MJ and Geisler C, 2017). It has been used for long-term therapy. Orlistat has been taken in conjugation with reduced-calorie diet. Fats soluble multivitamin can be taken before 2 hours or after taking orlistat. Orlistat gave rare or low side effects on liver (Amori RE, et al., 2007). In several randomized trials has been proved that orlistat with behavioral intervention gave better result in reduction of weight. It reduces 3 kg weight in comparison to placebo and behavioral intervention. According to (Xenical in the prevention of diabetes in obese subjects) trials it has been proved that orlistat with behavioral counseling leads to greater weight loss in 4 years of therapy. Among 3,305 patients during randomized study to orlistat or placebo, it was found that the group of orlistat lost 10.6 kg in 1 year and maintained a weight loss of 5.8 kg at 4 years, in comparison to group placebo 6.2 kg in 1 years and 3.0 kg-maintained weight loss in 4 years respectively (Blonde L and Jones RD, 2009).
Clinical use
120 mg capsule with each main meal has been recommended dose of orlistat for adults but should be omitted if a meal was missed. The patients should take, balanced diet which contain 30% calorie from fat (Buse JB, et al., 2009). But there are some benefits, adverse effects of orlistat (Figure 3).
Figure 3: Benefits, adverse effects and dosing of Orlistat
Drug increases energy consumption
Ephedrine and caffeine are the example of drug which increases energy consumption. During long term placebo-controlled clinical trial it has been showed that combination of these two drugs had more effects on obesity than when used alone. This substance has contained in some health supplements. But USFDA has not approved the combination of these two drugs for weight loss (Davies MJ, et al., 2015).
Anti-diabetic drugs
Liraglutide is glucagon-like peptide receptor agonist. It is a hormone secreted by intestinal cells. It stimulates the release of insulin and suppresses glucagon levels. It also reduces appetite and delays gastric emptying time. It has long half-life 13 hours. So, allowing given once daily. It has been approved by FDA for long term use (Ruifrok NAE, et al., 2009). Liraglutide at doses 1.2 mg and 1.8 kg mg daily reduces weight by 2.5 kg to 4 kg, but at dose 3.0 mg daily it has been approved for chronic weight management (Ruifrok NAE, et al., 2009). In the 56 week scale diabetes trials at dose 3.0 mg leads to reduction in 6 percent weight loss. Liraglutide also helps in improvement of fasting, post prandial glucose levels and fasting glucagon levels. It also reduces risk of cardiovascular problems. So, it is a greater choice of medicine patients having obesity, diabetes mellitus and cardiovascular diseases. This drug is best use with diet and proper exercise. Metformin, it is another example of anti-diabetic drug, insulin sensitizing agent from biguanide class. It works by increase in insulin sensitivity in peripheral tissue, reduces glucose production from liver. It also reduces glucose absorption from intestine and it does not increase insulin release. The half-life of metformin is 18 hours. At first prescribed at low dose and gradually increased to reach at optimal effect. Lactic acidosis was found to be a rare problem but it mainly occurs in diabetic patients having renal insufficiency. There are some research studies that prove it does not lead to much weight loss but significant weight loss has been observed. There are some other drugs used for long term medication approved by FDA (Tables 3 and 4).
| Drugs | Mechanism of action | Dose | Side effects | Weight loss |
|---|---|---|---|---|
| Lorcaserin | Activate serotonin5-HT2c receptor | 10 mg two times in a day | Headache, fatique, constipation, diabetes, hypoglycemia, backpain | 3.2 kg in 1 year |
| Liraglutide | Activate GLP1 receptor | 3 mg subcutaneously one times in a day | Nausea, vomiting, lipid level increases | 3-4 kg in 1 year |
| Phentermine- topiramate | Act on norepinephrine and GABA release | Phentermine 3.75 mg/Topiramate 23 mg once daily (loading dose) Phentermine 7.5 mg/Topiramate 46 mg once daily (maintenance dose) | Insomnia, paresthesia, dizziness, dysgeusia | 3.6 kg in 6 months |
| Naltrexone- bupropion | Inhibit Dopamine norepinephrine reuptake, block opioid receptor | 1 tab (bupropion 90 mg/naltrexone 8 mg) daily (loading dose and 2 tab (bupropion180 mg/naltrexone 16 mg) 2 times daily (maintenance dose) | Nausea, constipation, insomnia, drymouth diarrhea | 3.4 kg in 1 year |
| Diethylpropion | Act on central norepinephrine release | 25 mg 3 times in a day and 75 mg one time daily | Headache, insomnia, palpitation | 3 kg in 6 months |
Table 3: FDA approved drugs for treatment of obesity
| Drug | Year | Reason for banned |
|---|---|---|
| Dinitrophenol | 1938 | Dermatitis, neuropathy, agranulocytosis, visual impairment |
| Aminorex | 1968 | Chronic pulmonary hypertension |
| Amphetamine | 1971 | Addiction, hypertension, myocardial toxicity |
| Phenylpropanolamine | 2000 | Hemorrhagic stroke |
| Rimonabant | 2009 | Psychiatric disorders, depression, suicidal attempt |
| Sibutramine | 2010 | Risk of major cardiovascular events |
Table 4: List of banned drugs for obesity
Conclusion
The major step to improve the global health risk is awareness in people regarding obesity, its risk factors and how it can be reduced and management by several behavioral programmes such as physical activity diet plan, life style modification, and medicine. In early stage not only people but doctors play an important role in preventing obesity because in many rural areas and urban areas people concentrate more on doctor’s words. So, all physicians and family doctors should start promoting programs between patients to create a healthy country.
References
- Pozza C, Isidori AM. What’s behind the obesity epidemic? In imaging in bariatric surgery. Springer. 2018: 1-8.
- Kyrou I, Randeva HS, Tsigos C, Kaltsas G, Weickert MO, Feingold KR, et al. Clinical problems caused by obesity. Endotext. 2018.
- Ogden CL, Carroll MD, Fryar CD, Flegal KM. Prevalence of obesity among adults and youth: United States, 2011-2014. NCHS Data Brief. 2015.
- Calle EE, Rodriguez C, Thurmond WK, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl Med. 2003; 348(17): 1625-1638.
[Crossref] [Google scholar] [Pubmed]
- van Gaal LF, Mertens IL, de Block CE. Mechanisms linking obesity with cardiovascular disease. Nature. 2006; 444(7121): 875-880.
[Crossref] [Google scholar] [Pubmed]
- Mokdad AH, Ford ES, Bowman BA, Dietz WH, Vinicor F, Bales VS, et al. Prevalence of obesity, diabetes, andobesity-related health risk factors, 2001. JAMA. 2003; 289(1): 76-79.
[Crossref] [Google scholar] [Pubmed]
- Gadde KM, Allison DB. Combination therapy for obesity and metabolic disease. Curr Opin Endocrinol Diabetes Obes. 2009; 16(5): 353-358.
[Crossref] [Google scholar] [Pubmed]
- Jakobsen GS, Småstuen MC, Sandbu R, Nordstrand N, Hofsø D, Lindberg M, et al. Association of bariatric surgery vs. medical obesity treatment with long-term medical complications and obesity-related comorbidities. JAMA. 2018; 319(3): 291-301.
[Crossref] [Google scholar] [Pubmed]
- Obesity and overweight. World Health Organization (WHO). 2015.
- Obesity: Preventing and managing the global epidemic. Report of a WHO consultation. Geneva. World Health Organization (WHO). 1997.
- Han TS, Sattar N, Lean M. Assessment of obesity and its clinical implications. BMJ. 2006; 333(7570): 695-698.
[Crossref] [Google scholar] [Pubmed]
- Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults: The evidence report. Bethesda. National Heart, Lung and Blood Institute (NIH). 1998.
- Prevention and management of obesity (mature adolescents and adults). Institute for Clinical Systems Improvement (ICSI). 2011.
- Bray GA. Screening for and clinical evaluation of obesity in adults. UpToDate. 2013.
- Ghandehari H, Le V, Bahl KS, Wong ND. Abdominal obesity and the spectrum of global cardiometabolic risks in US adults. Int J Obes. 2009; 33(2): 239-248.
[Crossref] [Google scholar] [Pubmed]
- Healthy weight: Assessing your weight. Centers for Disease Control and Prevention (CDC). 2013.
- Westphal AB, Booke CA, Blocker T, Kossel E, Goele K, Later W, et al. Measurement site for waist circumference affects its accuracy as an index of visceral and abdominal subcutaneous fat in a Caucasian population. J Nutr. 2010; 140(5): 954-961.
[Crossref] [Google scholar] [Pubmed]
- Kannieappan LM, Deussen AR, Grivell RM, Yelland L, Dodd JM. Developing a tool for obtaining maternal skinfold thickness measurements and assessing inter-observer variability among pregnant women who are overweight and obese. BMC pregnancy childbirth. 2013; 13(1): 42.
[Crossref] [Google scholar] [Pubmed]
- Tarnoki AD, Tarnoki DL, Medda E, Cotichini R, Stazi MA, Fagnani C, et al. Bioimpedance analysis of body composition in an international twin cohort. Obes Res Clin Pract. 2014; 8(3): e291-7.
[Crossref] [Google scholar] [Pubmed]
- Report of the commission on ending childhood obesity. World Health organization (WHO). 2016.
- Ogden CL, Carroll MD, Lawman HG, Fryar CD, Moran KD, Kit BK, et al. Trends in obesity prevalence among children and adolescents in the United States, 1988-1994 through 2013-2014. JAMA. 2016; 315: 2292-2299.
[Crossref] [Google scholar] [Pubmed]
- Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of obesity among adults and youth: United States, 2015-2016. NCHS Data Brief. 2017; 288: 1-8.
[Google scholar] [Pubmed]
- Study on global ageing and adult health (SAGE). Geneva. World Health Organization (WHO). 2008.
- Global status report on non-communicable diseases 2014. World Health Organization (WHO). 2014.
- National Family Health Survey (NFHS-2), 1998-99. International Institute for Population Sciences (IIPS) and ORC Macro. 2000.
- National Family Health Survey (NFHS-3), 2005-06. International Institute for Population Sciences (IIPS) and ORC Macro. 2009.
- Devaux MG, Goryakin Y, Cecchini M, Huber H, Colombo F. OECD obesity update 2017. OECD. 2017.
- Frech HE, Miller RD. The effects of pharmaceutical consumption and obesity on the quality of life in the Organization of Economic Cooperation and Development (OECD) countries. Pharmacoeconomics. 2004; 22(2): 25-36.
[Crossref] [Google scholar] [Pubmed]
- Kaur S, Kapil U, Singh P. Pattern of chronic diseases amongst adolescent obese children in developing countries. Curr Sci. 2005; 88: 1052-1056.
- Palamara KL, Mogul HR, Peterson SJ, Frishman WH. New obesity perspectives and pharmacotherapies. Cardiol Rev. 2006; 14(5): 238-258.
[Crossref] [Google scholar] [Pubmed]
- The dietary guidelines for Americans 2005. US Department of Health and Human Services (USDA). 2008.
- Potter MB, Vu JD, Minihane CM. Weight management: What patients want from their primary care physicians. J Fam Pract. 2001; 50(6): 513-518.
[Google scholar] [Pubmed]
- Bray GA. Behavioral strategies in the treatment of obesity. UpToDate. 2013.
- LeBlanc ES, O’Connor E, Whitlock EP, Patnode CD, Kapka T. Effectiveness of primary care-relevant treatments for obesity in adults: Asystematic evidence review for the U.S. preventive services task force. Ann Intern Med. 2011; 15(7) 5: 434-447.
[Crossref] [Google scholar] [Pubmed]
- Rao G. Office-based strategies for the management of obesity. Am Fam Physician. 2010; 81(12): 1449-1456.
[Google scholar] [Pubmed]
- Searight HR. Realistic approaches to counseling in the office setting. Am Fam Physician. 2009; 79(4): 277-284.
[Google scholar] [Pubmed]
- Pollak KI, Alexander SC, Tulsky JA, Lyna P, Coffman CJ, Dolor RJ, et al. Physician empathy and listening: Associations with patient satisfaction and autonomy. J Am Board Fam Med. 2011; 24(6): 665-672.
[Crossref] [Google scholar] [Pubmed]
- Janssen I, LeBlanc AG. Systemic review of the health benefits of physical activity and fitness in school-aged children and youth. Int J Behav Nutr Phys Act. 2010. 7(1): 40.
[Crossref] [Google scholar] [Pubmed]
- Coleman KJ, Ngor E, Reynolds K, Virginia PQ, Corinna K, Rohm DB, et al. Initial validation of an exercise ‘vital sign’ in electronic medical records. Med Sci Sports Exerc. 2012; 44(11): 2071-2076.
[Crossref] [Google scholar] [Pubmed]
- 2008 physical activity guidelines for Americans. Office of disease prevention and health promotion (ODPHP). 2013.
- Rofey DL, Kolko RP, Iosif AM, Silk JS, Bost JE, Feng W, et al. A longitudinal study of childhood depression and anxiety in relation to weight gain. Child Psychiatry Hum Dev. 2009; 40: 517-526.
[Crossref] [Google scholar] [Pubmed]
- Anderson SE, Cohen P, Naumova EN, Jacques PF, Must A. Adolescent obesity and risk for subsequent major depressive disorder and anxiety disorder: Prospective evidence. Psychosom Med. 2007; 69: 740-747.
[Crossref] [Google scholar] [Pubmed]
- Bell JF, Zimmerman FJ. Shortened night time sleep duration in early life and subsequent childhood obesity. Arch Pediatr Adolesc Med. 2010; 164: 840-845.
[Crossref] [Google scholar] [Pubmed]
- Mcketta S, Rich M. The fault, dear viewer, lies not in thescreens, but in ourselves: Relationship between screen media and childhood overweight/obesity. Pediatr Clin North Am. 2011; 58: 1493-1508.
[Crossref] [Google scholar] [Pubmed]
- Andrews RA, Lim RB. Surgical management of severe obesity. UpToDate. 2013.
- SAGES Guidelines Committee. SAGES guideline for clinical application of laparoscopic bariatric surgery. Surg Obes Relat Dis. 2009; 5(3): 387-405.
[Crossref] [Google scholar] [Pubmed]
- Sjöström L, Narbro K, Sjöström CD, Karason K, Larsson B, Wedel H, et al. Effects of bariatric surgery on mortality in Swedishobese subjects. N Engl J Med. 2007; 357: 741-52.
[Crossref] [Google scholar] [Pubmed]
- Sjöström L, Peltonen M, Jacobson P, Sjostrom DC, Ksrason K, Wedel H, et al. Bariatric surgery and long-term cardiovascular events. JAMA. 2012; 307(1): 56-65.
[Crossref] [Google scholar] [Pubmed]
- Shah K, Nergard BJ, Frazier KS, Leifsson BG, Aghajani E, Gislason H. Long-term effects of laparoscopic Roux-en-Y gastric bypass on metabolic syndrome in patients with morbid obesity. Surg Obes Relat Dis. 2016; 12(8): 1449-1456.
[Crossref] [Google scholar] [Pubmed]
- Pucci A, Tymoszuk U, Cheung WH, Makaronidis JM, Scholes S, Tharakan G, et al. Type 2 diabetes remission 2 years post Roux‐en‐Y gastric bypass and sleeve gastrectomy: The role of the weight loss and comparison of DiaRem and DiaBetter scores. Diabet Med. 2018; 35(3):360-7.
[Crossref] [Google scholar] [Pubmed]
- Levine MS, Carucci LR. Imaging of bariatric surgery: Normal anatomy and postoperative complications. Radiology. 2014; 270(2): 327-341.
[Crossref] [Google scholar] [Pubmed]
- Novikov AA, Afaneh C, Saumoy M, Parra V, Shukla A, Dakin GF, et al. Endoscopic sleeve gastroplasty, laparoscopic sleeve gastrectomy, and laparoscopic band for weight loss: How do they compare. J Gastrointest Surg. 2018; 22(2): 267-273.
[Crossref] [Google scholar] [Pubmed]
- Goitein D, Raziel A, Szold A, Sakran N. Assessment of perioperative complications following primary bariatric surgery according to the Clavien-Dindo classification: comparison of sleeve gastrectomy and Roux-Y gastric bypass. Surg endosc. 2016; 30(1): 273-278.
[Crossref] [Google scholar] [Pubmed]
- Lara MD, Kothari SN, Sugerman HJ. Surgical management of obesity. Springer. 2005; 4(1): 55-64.
- Puzziferri N, Roshek TB, Mayo HG, Gallagher R, Belle SH, Livingston EH. Long-term follow-up after bariatric surgery: A systematic review. JAMA. 2014; 312(9): 934-942.
[Crossref] [Google scholar] [Pubmed]
- Snow V, Barry P, Fitterman N, Qaseem A, Weiss K. Pharmacologic and surgical management of obesity inprimary care: A clinical practice guideline from the American college of physicians. Ann Intern Med. 2005; 142(7): 525-531.
[Crossref] [Google scholar] [Pubmed]
- Leung WYS, Thomas GN, Chan JCN, Tomlinson B. Weight management and current options in pharmacotherapy: Orlistat and sibutramine. Clin Ther. 2003; 25(1): 58-80.
[Crossref] [Google scholar] [Pubmed]
- Kaplan LM. Pharmacologic therapies for obesity. Gastroenterol Clin North Am. 2010; 39: 6979.
[Crossref] [Google scholar] [Pubmed]
- Li MF, Cheung BMY. Rise and fall of anti-obesity drugs. World J Diabetes. 2011; 2(2): 1923.
[Crossref] [Google scholar] [Pubmed]
- Hendricks EJ. Off-label drugs for weight management. Diabetes Metab Syndr Obes. 2017; 10: 223.
[Crossref] [Google scholar] [Pubmed]
- Rebello CJ, Nikonova EV, Zhou S, Aronne LJ, Fujioka K, Garvey WT, et al. Effect of lorcaserin alone and in combination with phentermine on food cravings after 12‐week treatment: A randomized substudy. Obesity. 2018; 26(2): 332-339.
[Crossref] [Google scholar] [Pubmed]
- Bray GA. Use and abuse of appetite-suppressant drugs in the treatment of obesity. Ann Intern Med. 1993; 119: 707-713.
[Crossref] [Google scholar] [Pubmed]
- Henness S, Perry CM. Orlistat. Drugs. 2006; 66(12): 1625-1656.
[Crossref] [Google scholar] [Pubmed]
- Demos LL, Proietto J, Tonkin AM, McNeil JJ. Safety of drug therapies used for weight loss and treatment of obesity. Drug Saf. 2006; 29: 277-302.
[Crossref] [Google scholar] [Pubmed]
- Müller MJ, Geisler C. From the past to future: From energy expenditure to energy intake to energy expenditure. Eur J Clin Nutr. 2017; 71(3): 358-364.
[Crossref] [Google scholar] [Pubmed]
- Amori RE, Lau J, Pittas AG. Efficacy and safety of incretin therapyin type 2 diabetes: Systematic review and meta-analysis. JAMA. 2007; 298: 194-206.
[Crossref] [Google scholar] [Pubmed]
- Blonde L, Jones RD. The safety and efficacy of liraglutide with or without oral antidiabetic drug therapy in type 2 diabetes: An overview of the LEAD 1-5 studies. Diabetes Obes Metab. 2009; 11(suppl 3): 26-34.
[Crossref] [Google scholar] [Pubmed]
- Buse JB, Rosenstock J, Sesti G, Schmidt W, Montanya E, Brett JH, et al. Liraglutide once a day versus exenatide twice a day for type 2 diabetes: A 26-week randomized, parallel-group, multinational, open-label trial (LEAD-6). Lancet. 2009; 374: 39-47.
[Crossref] [Google scholar] [Pubmed]
- Davies MJ, Bergenstal R, Bode B, Kushner RF, Lewin A, Skjøth TV, et al. Efficacy of liraglutide for weight loss among patients with type 2 diabetes: The SCALE diabetes randomized clinical trial. JAMA. 2015; 314: 687-699.
[Crossref] [Google scholar] [Pubmed]
- Ruifrok NAE, Kuchenbecker WKH, Hoek A, Middleton P, Norman RJ. Insulin sensitizing drugs for weight loss in women of reproductive age who areoverweight or obese: Systematic review and meta-analysis. Hum Reprod Update. 2009; 15(1): 5768.
[Crossref] [Google scholar] [Pubmed]
Author Info
Meena Kedar Prasad*Citation: Prasad MK: New Trends Approach for Management of Obesity
Received: 14-Feb-2022 Accepted: 28-Feb-2022 Published: 10-Mar-2022, DOI: 10.31858/0975-8453.13.3.141-147
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3