Case Report - (2023) Volume 14, Issue 1
Abstract
Over the past 20 years, there has been a clear shift towards endovascular repair of the thoracic aorta in its various pathologies. However, complete endovascular repair of the aortic arch remains technically sophisticated. Currently, there are several methods of endovascular arch treatment: A hybrid approach, total endovascular debranching using parallel grafts (like a chimney or snorkeling) and fenestration (factory- made, hand-made (physician modified graft (PMG)) in-situ or outside (on-a-table)). The first results of the application of the aortic arch repair technology are promising, especially the complete replacement of the aortic arch be means of non-standard fenestrated or branched stent grafts. Use of fenestrated or branched grafts factory FTEVAR and Chimney is an attractive method for treating of aortic arch diseases but they have a higher cost and longer waiting time.
Keywords
Aortic dissection, Outside and in-situ, Fenestration, Aortic arch, Total arch, Stent-graft, FTEVAR, TEVAR
Introduction
A dissecting thoracic aortic aneurysm is urgent situation that requires close attention to surgical tactics aimed at preventing such serious complications as cardiac tamponade due to rupture of the intrapericardial part of the aorta and acute heart failure in severe aortic regurgitation. The incidence of aortic dissection is 5-10 cases per 100,000 population in the Russian Federation, from 0.2 to 0.8 per 100,000 population in the USA and from 0.5 to 2.95 cases per 100,000 population worldwide. Acute aortic dissection of type A (ORAA) is characterized by high mortality, which in the absence of treatment reaches up to 35% during the first 24 hours, 50% in 48 hours, from 80% to 94% in the 1st week. The mortality rate after aortic dissection is estimated at 1%-2% in 1 h.
Surgical treatment for the elimination of cardiac tamponade by eliminating the primary rupture and preventing further fatal complications. The choice of surgical method of correction of the proximal segment of the aorta depends on the experience of the surgeon and the technical capabilities of the clinic. Despite the limited data presented in the publication, several methods of performing graft fenestration with satisfactory short-term results have been described (Charchian ÉR, et al., 2014; Shket AP, et al., 2013; Mokashi SA and Svensson LG, 2019). We would like to present an example of several clinical cases of endovascular correction in acute pathology of the aortic arch and their results in an emergency medical clinic.
Case Presentation
First case (Gender: Female, 52 years old)
In March 2018, she was admitted to the Regional Emergency Center in Naberezhnye Chelny through the EMS channel with complaints of chest pain arising not directly connected with physical activity. It is known that in 2017, a supracoronary open ascending aorta repair was performed aortic dissection, type A (according to the Stanford classification). In 2018, due to the spread of dissection into the Left Common Carotid (LCC) and Left Subclavian Artery (LSA) and development of transitory ischemic attacks, we performed their stenting and subsequent Thoracic Endovascular Aortic Repair (TEVAR) of the descending aorta in Z3. Since October 2018 the patient began to have complaints of food-borne epigastric pains. In March 2019, control CT angiography revealed: Retrograde dissection of the thoracoabdominal aorta and aortic growth up to 6 mm and development of visceral artery malperfusion with spreading of dissection to the right common carotid artery (Figure 1).
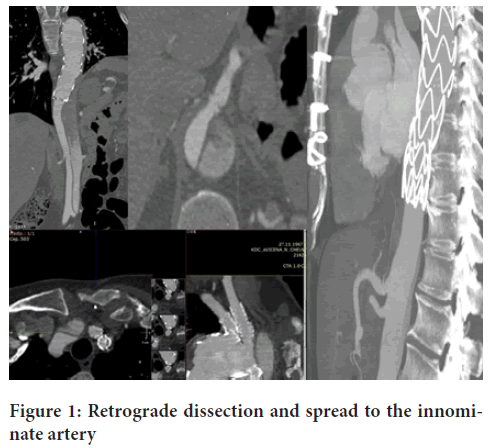
Figure 1: Retrograde dissection and spread to the innominate artery
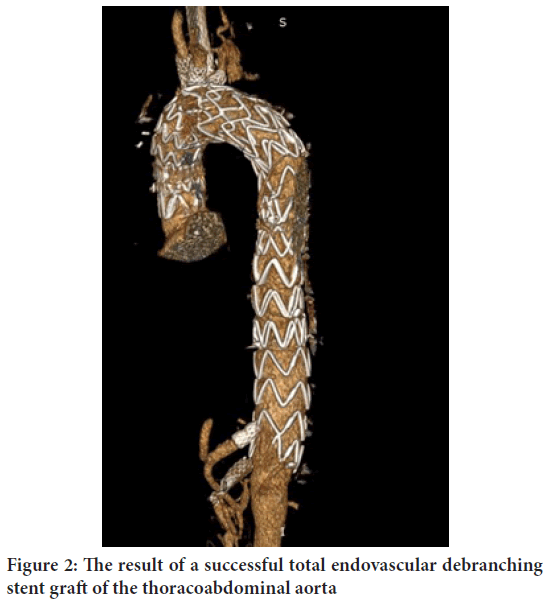
In this connection, we performed staged stenting of the right common carotid artery (RCCA) and TEVAR (first stage) using an in-situfenestration technique for the celiac trunk (by NBC-Technique) and stenting of the superior mesenteric artery. At the second stage, taking into account the aortic arch dissection and spread to the brachycephalic trunk (Figure 1), in June 2020, TEVAR was performed using “outside (on-a-table)” Fenestration Thoracic Endovascular Aortic Repair (FTEVAR) of the aortic arch with stenting of the right common carotid and right subclavian arteries (Figure 2) .
Figure 2: The result of a successful total endovascular debranching stent graft of the thoracoabdominal aorta
Second case (Gender: Male, 37 years old)
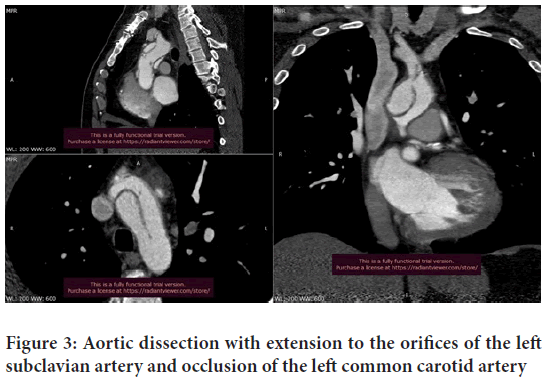
In December 2020 patient was admitted to the Regional Emergency Center in Naberezhnye Chelny on an emergency call with pain syndrome of the interscapular region and a Syncopal episode. According to the clinic and CT angiography, the diagnosis was: Type A dissection (according to Stanford classification) with dissection spread to the brachiocephalic (Innominate artery, LCCA, LSA) arteries complicated by cerebral malperfusion syndrome (Figure 3). According to echocardiogram, the aortic valve insufficiency of 2-3 grade was revealed.
Results and Discussion
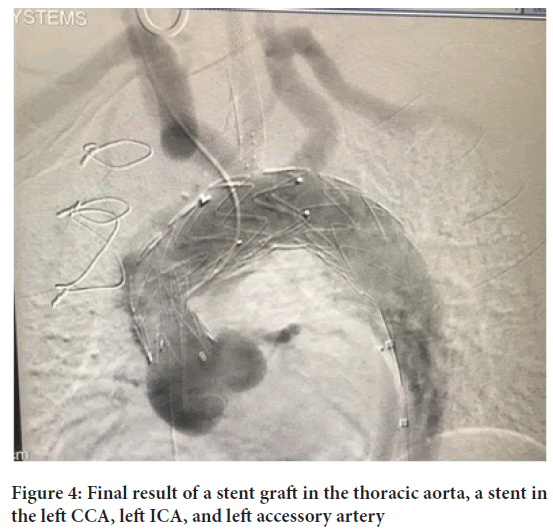
A life-saving supracoronary prosthetics with simultaneous CABG to obtuse marginal artery was performed under hypothermia (28°C). At the second stage stenting of the left ICA was performed. The patient was discharged from the hospital in satisfactory condition 10 day after without neurological deficits. 8 months later, control CT angiography: Dissection remains at the level of the aortic arch branches (Figure 3). Therefore, we performed FTEVAR using wide fenestration under the aortic arch arteries, the “outside on-a-table” technique, followed by their stenting. Thus, a “landing zone” was created for the subsequent graft into the descending thoracic aorta from the mouth of the left CCA, as well as this “in-situ” graft fenestration was performed under the left common carotid artery followed insertion of a stent (Figure 4). Thus, in two cases presented a total endovascular repair of the aortic arch (total arch) was performed using the new “outside” (on-a-table) and “in-situ” fenestration technology. Longer studies are needed to assess the durability and effectiveness this innovative endovascular procedure.
Figure 3: Aortic dissection with extension to the orifices of the left subclavian artery and occlusion of the left common carotid artery
Figure 4: Final result of a stent graft in the thoracic aorta, a stent in the left CCA, left ICA, and left accessory artery
Our experience in the use of aortic arch endoprosthetics with use of “outside” and “in-situ” fenestration techniques for pathologies has shown encouraging results with low mortality and frequency of complications, which indicates that these methods of minimally invasive treatment are safe and feasible (Zhang J, et al., 2020; Moulakakis KG, et al., 2013; Glorion M, et al., 2016). Due to low trauma, there was a reduction in the length of stay in the hospital. F-TAVAR is a promising and more reasonable method used to repair the aorta without changing anatomical structures. In our practice, we took advantage of the characteristics of various stent graft, which made the planning, modification and orientation procedures much more efficient and effective. In our experience with endoprosthetics of the aortic arch using the “outside” and “in-situ” fenestration technique, only two out of 48 (4.16%) patients developed endolic, which is consistent with recent publications that reported the frequency of endolic 0%-4.2% (Shu C, et al., 2020).
Thus, based on the individual advantages and limitations, as well as the encouraging results of these methods in the early and medium term, each of the methods can be applied in endovascular surgery (Makaloski V, et al., 2018). Given the significant limitation of the study in the form of a small number of patients and follow-up time, we consider it necessary to conduct further long-term follow-up in a large cohort of patients (Canaud L, et al., 2017; Zhu J, et al., 2018).
Conclusion
Surgical treatment with circulatory arrest and hypothermia remains the gold standard in the treatment of aortic arch pathology, but it is a technically more sophisticated and traumatic operation associated with a high risk of complications and mortality. For this reason, we have proposed a new method hand-made (physician modified graft (PMG)) FTEVAR in case of type. An aortic dissection with graft fenestration using “outside” and “in-situ” techniques. Our Regional Emergency Center was the first in the Russian Federation to use this type of treatment in 13 patients with follow-up for more than 52 months. We have also developed an optimal drug therapy management.
Authors Contribution
Akhmedov U and Sharafutdinov M-Concept and design of the article, literature review; Sharafutdinov M, Yakubov R-Correction of the article; Akhmedov U, Khairutdinov A, Tarasov Yu, Sadykov R-Review and analysis of data.
References
- Charchian ÉR, IuV B, Stepanenko AB, Gens AP, Fedulova SV, RIu N. Valve-sparing technique for type a aortic dissection with insufficiency of aortic valve. Kardiologiia. 2014; 54(6): 91-96.
[Crossref] [Google scholar] [Pubmed]
- Shket AP, Shumovets VV, Spiridonov S V. The experience of surgical treatment of thoracic dissecting aneurisms of a type. Medical Almanac. 2013: 4(28): 65-67.
- Mokashi SA, Svensson LG. Guidelines for the management of thoracic aortic disease in 2017. Gen Thorac Cardiovasc Surg. 2019; 67(1): 59-65.
[Crossref] [Google scholar] [Pubmed]
- Zhang J, Liu X, Tian M, Chen H, Wang J, Ji M, et al. Endovascular aortic repairs combined with looping-chimney technique for repairing aortic arch lesions and reconstructing left common carotid artery. J Thorac Dis. 2020; 12(5): 2270.
[Crossref] [Google scholar] [Pubmed]
- Moulakakis KG, Mylonas SN, Markatis F, Kotsis T, Kakisis J, Liapis CD. A systematic review and meta-analysis of hybrid aortic arch replacement. Ann Cardiothorac Surg. 2013; 2(3): 247.
[Crossref] [Google scholar] [Pubmed]
- Glorion M, Coscas R, McWilliams RG, Javerliat I, Goëau-Brissonniere O, Coggia M. A comprehensive review of in situ fenestration of aortic endografts. Eur J Vasc Endovasc Surg. 2016; 52(6): 787-800.
[Crossref] [Google scholar] [Pubmed
- Shu C, Fan B, Luo M, Li Q, Fang K, Li M, et al. Endovascular treatment for aortic arch pathologies: Chimney, on-the-table fenestration, and in-situ fenestration techniques. J Thorac Dis. 2020; 12(4): 1437.
[Crossref] [Google scholar] [Pubmed]
- Makaloski V, Tsilimparis N, Rohlffs F, Heidemann F, Debus ES, Kölbel T. Endovascular total arch replacement techniques and early results. Ann Cardiothorac Surg. 2018; 7(3): 380.
[Crossref] [Google scholar] [Pubmed]
- Canaud L, Baba T, Gandet T, Narayama K, Ozdemir BA, Shibata T, et al. Physician-modified thoracic stent-grafts for the treatment of aortic arch lesions. J Endovasc Ther. 2017; 24(4): 542-548.
[Crossref] [Google scholar] [Pubmed]
- Zhu J, Zhao L, Dai X, Luo Y, Fan H, Feng Z, et al. Fenestrated thoracic endovascular aortic repair using physician modified stent grafts for acute type B aortic dissection with unfavourable landing zone. Eur J Vasc Endovasc Surg. 2018; 55(2): 170-176.
[Crossref] [Google scholar] [Pubmed]
Author Info
Akhmedov U*, Sharafutdinov M, Yakubov R, Sadykov R, Khairutdinov A and Tarasov YuCitation: Akhmedov U: Total Aortic Arch Endoprosthetic Repair using the �¢??Outside�¢?� and �¢??In-Situ�¢?� Fenestration Techniques: First Results in Russia
Received: 02-Dec-2022 Accepted: 27-Dec-2022 Published: 03-Jan-2023, DOI: 10.31858/0975-8453.14.1.38-40
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3