Research Article - (2023) Volume 14, Issue 6
Abstract
This article presents data of incidence, cause and other knowledge we have about non cutaneous melanomas. What we found is that when analyzing cases with this type of cancer in Asturias, the incidence is much higher than what it is described in the literature for other parts of the world. It is interesting because the study has been carried out in the Central hospital of Asturias; it is the reference hospital in this province of northern Spain. My opinion is that the life expectancy of the region, combined with the lifestyle we have in Asturias, influences these data in a very noticeable way.
Keywords
Uveal melanoma, Mucosal melanoma, Non-cutaneous melanoma
Introduction
The development of melanoma is due to uncontrolled proliferation of melanocytes, which are responsible for pigment production. About 90% of melanoma cases are cutaneous melanoma. Non cutaneous subtypes include uveal and mucosal melanoma (Sánchez RB, et al., 2015).
Mucosal melanoma accounts for less than 1% of all malignant melanomas, but is one of the most aggressive subtypes and, because of that the prognosis is worse compared to common cutaneous melanoma. As the incidence of cutaneous melanoma is increasing, the incidence of mucosal melanoma remains stable. The highest incidence of mucosal melanoma is found in the head and neck region (55.4%), followed by anus and rectum (23.8%), female reproductive urinary tract (18%) and mucosa of the urinary tract (2.8%) (Sánchez RB, et al., 2015; Olla D and Neumeister MW, 2021; Goldemberg DC, et al., 2019).
The median age of diagnosis is 70 years for mucosal melanoma, decades later than for cutaneous melanomas (Olla D and Neumeister MW, 2021).
Sixty-five percent of patients are over the age of 60, and less than 3% are under the age of 30. Mucosal melanoma is twice as common in women. Female predominance is more evident given a higher rate of melanomas of the genital tract, while there are no differences in rates between sexes for extra-genital mucosal melanoma (Olla D and Neumeister MW, 2021).
Compared to a 5-year survival rate of 80.8% in cutaneous melanomas, mucosal melanoma has a 5-year survival of only 25% (Olla D and Neumeister MW, 2021; Goldemberg DC, et al., 2019; Ma Y, et al., 2021).
The biology of mucosal melanocytes and the risk factors that are related to the incidence of mucosal melanoma is not very studied, so, the prognosis and survival in this type of cancer is worse than in others melanomas.
Antimicrobial and immunologic cellular functions are proposed for the function of melanocytes in the mucosal membranes because is not well understood (Olla D and Neumeister MW, 2021).
“UV exposure is a well-established risk factor for cutaneous melanoma, but the mutagens that contribute to the development of mucosal melanoma remain unknown. According to epidemiological studies, smoking, inadequate dentures and ingested/ inhaled carcinogens such as tobacco and formaldehyde are considered potential causal factors for oral route and melanoma of the Sino nasal mucosa, while chronic inflammatory disease, viral infections and chemical irritants are thought to be involved in melanoma of the vulvar mucosa. Human Immunodeficiency Virus (HIV) is associated with anorectal and mucosal melanoma” (Ma Y, et al., 2021).
Mucosal melanoma differs from cutaneous melanoma in terms of epidemiology, genetic profile, clinical presentation, and response to therapies. Although there are differences, mucosal melanomas are generally treated in the same way as cutaneous melanomas. It has been seen that patients with mucosal melanoma exhibit a lower response rate to immunotherapy than patients with cutaneous melanomas, survival in the first group is lower (Santeufemia DA, et al., 2023).
Surgical resection with clear margins is the mainstay treatment, but this is influenced by the size of the tumor, proximity to vital structures, functional considerations, and anatomic complexity (Olla D and Neumeister MW, 2021).
Cutaneous melanoma is mainly classified into 4 genomic subtypes: BRAF (52%), RAS (31%), NF1 (14%) and a small portion of wild triple type. Therefore, co-targeted guidance to BRAF and MEK has been shown to achieve a significant response rate for BRAF V600 in cm patients in clinical management” (Ma Y, et al., 2021).
In contrast, mucosal melanoma has more diverse mutation patterns, with less than 20% of BRAF V600E mutations, followed by most scattered and difficult mutations difficult to attack, including NRAS, NF1, KIT, SF3B1 and SPRED1 (Ma Y, et al., 2021).
Uveal melanoma is the most common eye cancer in adults with an incidence of 5 cases per million individuals annually in the United States (Fallico M, et al., 2021).
The 90%-95% of uveal melanomas is found in the choroid. The diagnosis is based on clinical examination and other test as ultrasonography (that can be very valuable when it is found an indeterminate choroidal lesion). Studying these cases can be useful when documenting.
The treatment begins with biopsy using a fine needle aspiration with a prognostic purpose in combination with radiotherapy. Depending on the genetic result of this biopsy, a multidisciplinary treatment is used for these patients.
Primary tumor treatment can be enucleation or globe preserving. Usually, enucleation is used when the tumor is large and radiotherapy is preferred for small/medium melanomas.
The tendency to metastasize is high and the prognosis is unfavorable due to the high mortality rate that increase 80% in one year because of the absence of an effective treatment and the aggressiveness of the condition.
Novel molecular studies have allowed for a better understanding of the genetic and epigenetic mechanisms involved in uveal melanoma biological activity, which differs compared to skin melanomas. The most commonly mutated genes are GNAQ, GNA11 and BAP1 (Fallico M, et al., 2021).
It should be noted that patients affected with uveal melanoma are approximately ≥ 11% more likely to develop secondary cancer than the rest of the population, including: Renal cell carcinoma and cutaneous melanoma, which may be related to the BAP1 germline. Research into this gene could help identify diagnoses and biomarkers, as well as new therapeutic targets (Fallico M, et al., 2021).
Host susceptibility factors related to the formation of this cancer are as follows: Race or ethnicity-White, clear eyes, fair skin, skin that tans.
Materials and Methods
Consulting the patients diagnosed with melanoma in the hospital Central Oviedo registry of tumors between January 2010 and December 2020, we see that from 348 patient with melanoma, 51 patients were non-cutaneous melanomas (14.66%), of which 16 corresponded to mucosal melanomas (4.6%) and 35 to uveal melanomas (10.6%). The study makes sense since the central hospital of Oviedo is the reference in the Principality of Asturias. Therefore, we obtain a very representative data of these types of cancers in the region
The medical records of all patients in the study were reviewed in computer support (through the Health History of the Principality of Asturias, Millenium), to obtain the following data:
We studied 51 patients affected by mucosal and uveal melanoma, 23 men (45.1%) and 28 women (54.9%)
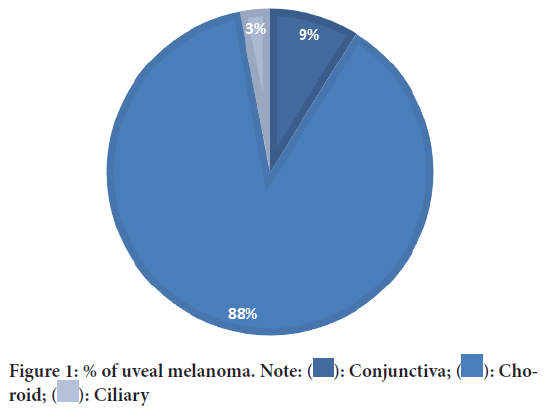
1. Uveal melanoma (Figure 1)-
Figure 1: % of uveal melanoma. Note:  : Conjunctiva;
: Conjunctiva;  : Choroid;
: Choroid;  : Ciliary
: Ciliary
• Choroid: 85.71%
• Conjunctiva: 8.57%
• Ciliary: 2.86%
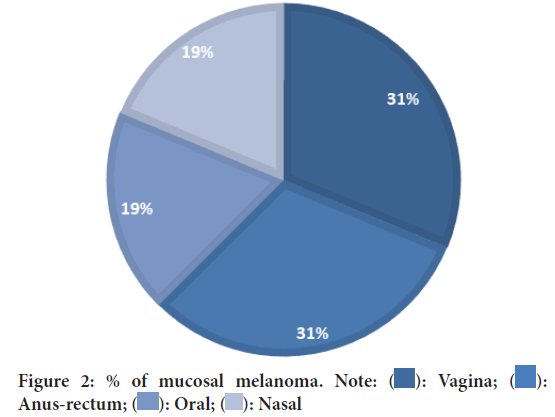
2. Mucosal melanomas (Figure 2)-
Figure 2: % of mucosal melanoma. Note:  : Vagina;
: Vagina;  : Anus-rectum;
: Anus-rectum;  : Oral;
: Oral;  : Nasal
: Nasal
• Vagina: 31.25%
• Anus-rectum: 31.25%
• Oral: 18.75%
• Nasal: 18.75%
In a previous study patients diagnosed with primary cutaneous melanoma at the Central University Hospital of Asturias Hospital in Oviedo during the period between January 1, 2008 and December 31, 2012 were selected from the database of the Hospital Registry of Tumors. Total 275 patients in which 175 women (62.5%) and 100 men (37.5%) with mean age of 64.9 years at diagnosis.
The annual number of cases nearly doubled from the beginning to the end of the study period. 37.5% of patients were referred, incorrectly, at a normal rate, so it is convenient to improve the referral process. Women developed melanoma much more often than men, while men with melanoma developed non-melanoma skin cancer more often. The average age was much higher than that observed in other regions of Spain. The elderly patients debuted with melanomas significantly thicker than the rest of the patients. Significant factors with a worse prognosis were age, Breslow thickness >2 mm, ulceration, presence of metastases, and stages III and IV (Seral CM, 2017).
As we can see, cases of melanomas in Asturias are increasing since 2008 and, the percentages of incidence in or Asturias sample are relatively higher than the data that are published in American studies where it seen that the incidence of mucosal melanomas is around 1% of cases of melanoma and uveal represent 4% of total cases (Goldemberg DC, et al., 2019; Ma Y, et al., 2021; Fallico M, et al., 2021; Vergara IA, et al., 2022).
Results and Discussion
The data we have for melanomas in Asturias are from 2008 to 2020 and those on non-cutaneous melanoma are from 2020, we can be guided by the general cancer data to draw conclusions about why the incidence of these types of cancers is higher than in other parts of the world.
Asturias is one of the autonomous communities in which the incidence of cancer is highest: But the Spanish Association against Cancer (AECC) revealed on the day that World Cancer Day was commemorated in 2023, that Asturias is the community with the highest crude rate of new cancer cases, with a figure of 765 per 100,000 inhabitants. The cause is that most tumor diseases manifest themselves over 60 years of age and Asturias is one of the communities with the oldest population in the country.
Asturias has particularities of aging population and decline in the register. According to the dynamic report of the AECC, if the crude rate of new detected cases of cancer in 2022 stood at 765 cases per 100,000 inhabitants, the crude rate is estimated to rise to 798 in 2025, 861 in 2023, 923 in 2035 and 969 in 2040.
As we can see, age is an important factor when it comes to developing cancer. In recent years life expectancy has increased and that explains why we have more patients of developing age of Cancer. As indicated by the SEOM report, from the age of 45-50 there is a risk of cancer of 40.9% in men and 27.6% in women. At age 85, these values are 48.6% in men and 32.2% in women.
Every year around 7600 new cases of cancer are detected in the principality according to the Spanish Association against Cancer (AECC).
The Spanish Society of Medical Oncology (SEOM) has presented in February 2022 the data of the report cancer in Spain in 2022, in which 280,100 new cases are expected to be diagnosed, with a greater predominance in men (166,066) than in women (120,035). In 2022, according to this estimate, there will be a slight increase compared to 2021, when a total of 276,000 cases were diagnosed, experts have warned that it should be understood how the incidence of COVID has influenced these data because during 2020 and 2021 patient went less to the hospitals.
As for survival, the report presented in February by the SEOM Cancer in Spain in 2022, argues that cancer deaths are associated with five factors that can be prevented. Tobacco is responsible for up to 22 percent of deaths. It has also revealed other factors such as alcohol intake or obesity.
According to WHO data, in Spain 4.4% of tumors are directly caused by alcohol. Europe has one of the highest levels of alcohol consumption globally. According to the SEOM in its report, there is no safe level of alcohol consumption. In addition, there is a synergy with the habit of smoking, and is that when alcohol and tobacco consumption are combined, the risk of developing oral, oropharyngeal or esophageal carcinomas multiplied by 30.
As for obesity, it is estimated that if the average population Body Mass Index (BMI) worldwide had not increased in the last 30 years, more than 160,000 cases of cancer could have been avoided in 2012 worldwide.
The Nutritional Study of the Spanish Population (ENPE) shows that 53.6% of Spaniards are obese or overweight. This new data have been published in ‘Revista Española de Cardiología’ (REC), the main header of REC Publications, the family of scientific publications of the Spanish Society of Cardiology (SEC). Thus, 22% of Spaniards have obesity, with no differences between men and women, and 31.6% are overweight, this being significantly higher in men.
The autonomous communities with the highest obesity rates in Spain are Andalusia and Galicia (26.7%), followed by the Principality of Asturias (26.2%) and the Region of Murcia (25.7%). The Balearic Islands (11.7%), Catalonia (16.1%) and the Basque Country (16.5%) have the lowest obesity rates.
As new treatments we talk about biomarkers, they allow us to subdivide and classify tumors, as well as select the most effective and safe treatments for patients. The Ministry of Health is working on updating the portfolio of services in the genetic area so that it can be implemented quickly and globally in Spain.
Conclusion
With all these data, we can conclude that the high percentage of the population that smokes in Asturias (19.2% according to data from the National Institute of Statistics in May 2022), the obesity and the high alcohol consumption of the principality (21.1% of the population-data of January 2022) are contributing, together with the high life expectancy of the population, more cancers develop in non-cutaneous melanomas as well as in other types of cancers than in the rest of the world.
References
- Sánchez RB, de Unamuno Bustos B, Mira MN, Estrada RB. Actualización en melanoma mucoso. Actas Dermosifiliogr. 2015; 106(2): 96-103.
[Crossref] [Google scholar] [PubMed]
- Olla D, Neumeister MW. Mucosal melanoma. Clin Plast Surg. 2021; 48(4): 707-711.
[Crossref] [Google scholar] [PubMed]
- Goldemberg DC, Thuler LCS, de Melo AC. An update on mucosal melanoma: Future directions. Acta Dermatovenerol Croat. 2019; 27(1): 11-15.
[Google scholar] [PubMed]
- Ma Y, Xia R, Ma X, Judson-Torres RL, Zeng H. Mucosal melanoma: Pathological evolution, pathway dependency and targeted therapy. Front Oncol. 2021; 11: 702287.
[Crossref] [Google scholar] [PubMed]
- Santeufemia DA, Palmieri G, Miolo G, Colombino M, Doro MG, Frogheri L, et al. Current trends in mucosal melanomas: An overview. Cancers. 2023; 15(5): 1356.
[Crossref] [Google scholar] [PubMed]
- Fallico M, Raciti G, Longo A, Reibaldi M, Bonfiglio V, Russo A, et al. Current molecular and clinical insights into uveal melanoma. Int J Oncol. 2021; 58(4): 1-.
[Crossref] [Google scholar] [PubMed]
- Seral CM. Estudio clínico patológico del melanoma cutáneo en el Hospital Universitario Central de Asturias (periodo 2008-2012). Repositorio Institucional de la Universidad de Oviedo. 2017.
- Vergara IA, Wilmott JS, Long GV, Scolyer RA. Genetic drivers of non‐cutaneous melanomas: Challenges and opportunities in a heterogeneous landscape. Exp Dermatol. 2022; 31(1): 13-30.
[Crossref] [Google scholar] [PubMed]
Author Info
Mar�a Teresa Sotelo-Luina*Citation: Systematic Review Pharmacy Sotelo-Luina MT: Trends in the Incidence of Mucosal and Uveal Melanoma in Asturias
Received: 08-May-2023 Accepted: 02-Jun-2023 Published: 09-Jun-2023, DOI: 10.31858/0975-8453.14.6.380-382
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
ARTICLE TOOLS
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Psychometric properties of the World Health Organization Quality of life instrument, short form: Validity in the Vietnamese healthcare context Trung Quang Vo*, Bao Tran Thuy Tran, Ngan Thuy Nguyen, Tram ThiHuyen Nguyen, Thuy Phan Chung Tran SRP. 2020; 11(1): 14-22 » doi: 10.5530/srp.2019.1.3
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- Deuterium Depleted Water as an Adjuvant in Treatment of Cancer Anton Syroeshkin, Olga Levitskaya, Elena Uspenskaya, Tatiana Pleteneva, Daria Romaykina, Daria Ermakova SRP. 2019; 10(1): 112-117 » doi: 10.5530/srp.2019.1.19
- Dental Development between Assisted Reproductive Therapy (Art) and Natural Conceived Children: A Comparative Pilot Study Norzaiti Mohd Kenali, Naimah Hasanah Mohd Fathil, Norbasyirah Bohari, Ahmad Faisal Ismail, Roszaman Ramli SRP. 2020; 11(1): 01-06 » doi: 10.5530/srp.2020.1.01
- Manilkara zapota (L.) Royen Fruit Peel: A Phytochemical and Pharmacological Review Karle Pravin P, Dhawale Shashikant C SRP. 2019; 10(1): 11-14 » doi: 0.5530/srp.2019.1.2
- Pharmacognostic and Phytopharmacological Overview on Bombax ceiba Pankaj Haribhau Chaudhary, Mukund Ganeshrao Tawar SRP. 2019; 10(1): 20-25 » doi: 10.5530/srp.2019.1.4
- A Review of Pharmacoeconomics: the key to “Healthcare for All” Hasamnis AA, Patil SS, Shaik Imam, Narendiran K SRP. 2019; 10(1): s40-s42 » doi: 10.5530/srp.2019.1s.21
- A Prospective Review on Phyto-Pharmacological Aspects of Andrographis paniculata Govindraj Akilandeswari, Arumugam Vijaya Anand, Palanisamy Sampathkumar, Puthamohan Vinayaga Moorthi, Basavaraju Preethi SRP. 2019; 10(1): 15-19 » doi: 10.5530/srp.2019.1.3